Parathyroid Glands & PTH Regulation of Calcium, Phosphate and Bone Homeostasis
The parathyroid glands are small but critically important endocrine organs located on the posterior surface of the thyroid gland. Their primary function is the regulation of extracellular calcium and phosphate levels through the secretion of parathyroid hormone (PTH). Calcium homeostasis is essential for neuromuscular excitability, blood clotting, enzyme function and bone integrity. Because fluctuations in calcium levels can have immediate and life-threatening consequences, PTH secretion is tightly regulated and highly responsive to even subtle changes in plasma calcium concentration.
What You Need to Know
The parathyroid glands play a critical role in maintaining calcium and phosphate balance through the secretion of parathyroid hormone (PTH). PTH is released in response to falling serum calcium levels and acts rapidly to restore calcium concentration within a narrow physiological range. Because calcium is essential for neuromuscular excitability, cardiac conduction, blood coagulation, and bone integrity, this regulation is tightly controlled.
PTH acts on multiple target organs to increase circulating calcium while simultaneously reducing phosphate levels. Its effects are coordinated rather than isolated, ensuring that calcium availability is increased without promoting pathological calcium–phosphate precipitation in tissues.
The key actions of PTH include:
bone, where PTH stimulates calcium release by increasing bone resorption
kidney, where it enhances calcium reabsorption, increases phosphate excretion, and stimulates activation of vitamin D
gastrointestinal tract, indirectly, where activated vitamin D increases intestinal absorption of calcium
These mechanisms restore serum calcium levels and maintain long-term mineral homeostasis. Through its integrated actions on bone, kidney, and gut, PTH links skeletal health to renal function and intestinal absorption, ensuring stable plasma calcium levels despite variations in dietary intake or physiological demand.
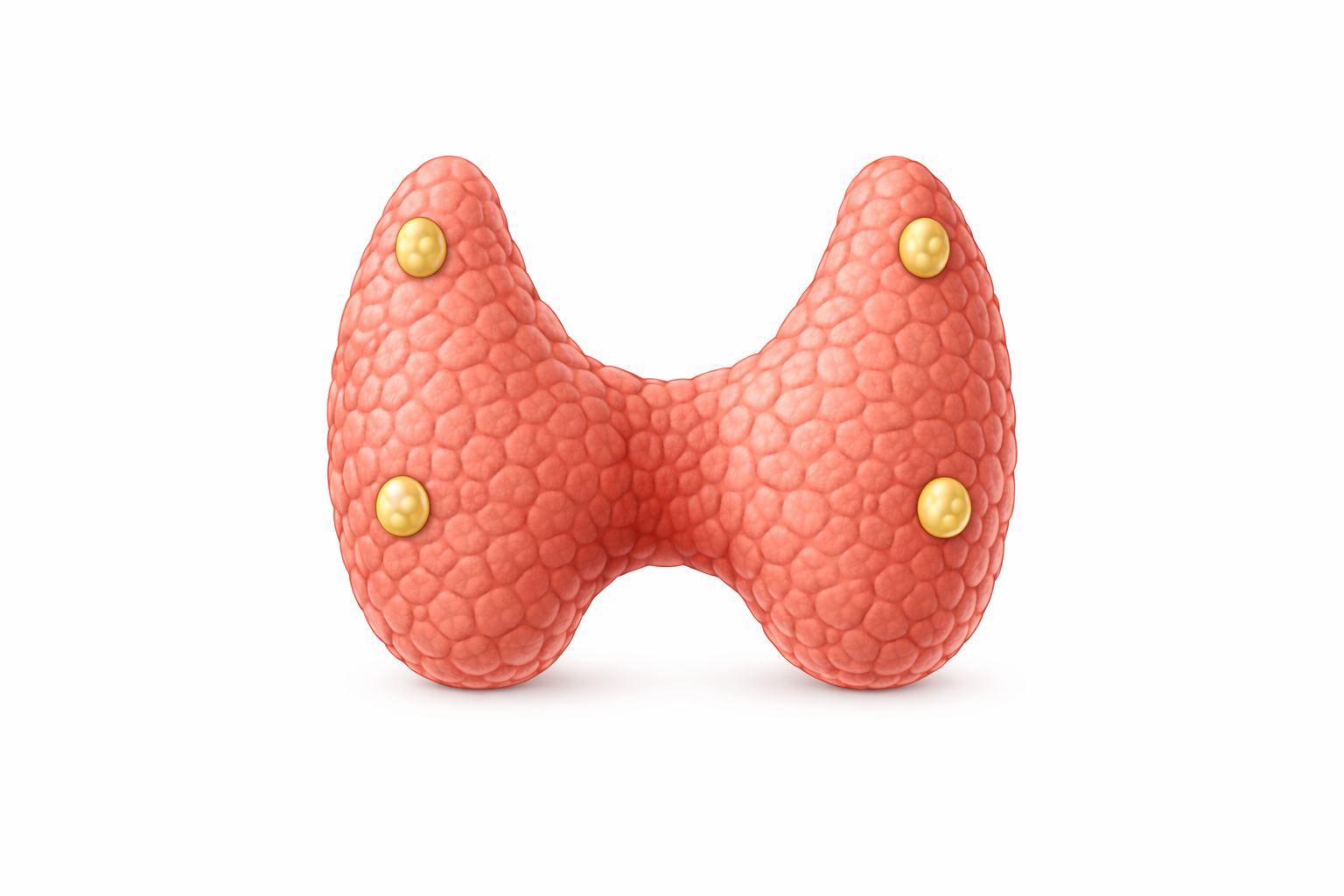
Image: Posterior view of the thyroid gland. The parathyroid glands are typically (the actual number can vary) four small endocrine glands located on the posterior surface of the thyroid. Their position can vary, but they are usually found embedded along its back surface. Despite their size, they play a critical role in calcium homeostasis through secretion of parathyroid hormone (PTH).
Beyond the Basics
Calcium-sensing receptors and real-time regulation
Chief cells of the parathyroid glands express calcium-sensing receptors (CaSR) that continuously monitor circulating ionised calcium. When serum calcium falls, these receptors detect the change almost immediately and trigger rapid PTH release, allowing correction of calcium levels within minutes rather than hours. This direct sensing mechanism makes the parathyroid glands one of the fastest-responding endocrine systems in the body and allows calcium homeostasis to be regulated on a moment-to-moment basis rather than through delayed hormonal cascades.
When calcium levels rise, activation of CaSR suppresses PTH secretion, preventing excessive calcium accumulation in the circulation. This tight feedback loop maintains plasma calcium within a very narrow physiological range despite fluctuations in dietary intake, renal excretion, or skeletal demand.
PTH actions on bone
Parathyroid hormone does not act directly on osteoclasts but instead influences bone through osteoblast signalling. PTH stimulates osteoblasts to increase expression of receptor activator of nuclear factor kappa-B ligand (RANKL), which promotes osteoclast differentiation and activation. The resulting increase in osteoclast-mediated bone resorption releases calcium and phosphate into the bloodstream, providing a rapid source of mineral when extracellular calcium levels fall.
The pattern of PTH exposure is physiologically critical. Sustained elevation of PTH favours net bone resorption and contributes to cortical bone loss, as seen in hyperparathyroidism. In contrast, brief, intermittent PTH exposure preferentially stimulates osteoblast activity and bone formation. This distinction explains why intermittent PTH analogues are used therapeutically to treat osteoporosis, while chronic PTH excess weakens the skeleton.
PTH effects on the kidney
The kidney is a major effector organ for PTH and plays a central role in fine-tuning calcium and phosphate balance. PTH increases calcium reabsorption in the distal nephron, reducing urinary calcium loss at times of deficiency. At the same time, it decreases phosphate reabsorption in the proximal tubule, increasing phosphate excretion and preventing excessive calcium–phosphate product formation in the circulation, which could otherwise promote pathological calcification.
PTH also stimulates renal 1α-hydroxylase activity, converting inactive vitamin D into its biologically active form, calcitriol. This step links renal function directly to intestinal calcium absorption and highlights why kidney disease profoundly disrupts mineral metabolism even when parathyroid glands are intact.
Interaction with vitamin D
Parathyroid hormone and vitamin D function as an integrated regulatory system rather than as isolated hormones. Falling calcium levels stimulate PTH release, PTH activates vitamin D in the kidney, and active vitamin D increases intestinal absorption of calcium, restoring extracellular calcium levels. As calcium normalises, PTH secretion falls, completing the feedback loop.
Disruption at any point in this pathway alters the entire system. Vitamin D deficiency, impaired renal activation, or parathyroid dysfunction all lead to compensatory changes in PTH secretion and characteristic patterns of calcium and phosphate disturbance. Understanding this interdependence is essential for interpreting laboratory abnormalities and recognising whether bone, kidney, gut, or endocrine pathology is driving the imbalance.
Clinical Connections
Disorders of parathyroid hormone secretion produce characteristic and clinically important patterns of calcium and phosphate imbalance. Because PTH sits at the centre of bone, kidney, and vitamin D regulation, abnormalities in its secretion or action have widespread systemic effects that are often multisystem in presentation.
Primary hyperparathyroidism, most commonly caused by a parathyroid adenoma, is characterised by autonomous PTH secretion despite elevated serum calcium. Persistently high PTH drives excessive bone resorption, increases renal calcium reabsorption, and enhances vitamin D activation, resulting in hypercalcaemia. Clinical manifestations reflect these mechanisms and commonly include skeletal fragility, nephrolithiasis, gastrointestinal symptoms such as constipation, and neuropsychiatric changes including fatigue, low mood, and cognitive slowing.
Secondary hyperparathyroidism arises as a compensatory response rather than a primary gland disorder. It is most often seen in chronic kidney disease, where reduced renal activation of vitamin D and phosphate retention lower serum calcium and stimulate sustained PTH release. Although initially adaptive, prolonged elevation of PTH contributes to renal osteodystrophy, vascular calcification, and disordered mineral metabolism, even when serum calcium is normal or low.
Hypoparathyroidism, most commonly following thyroid or parathyroid surgery, results from insufficient PTH secretion. Reduced PTH leads to hypocalcaemia, impaired renal calcium reabsorption, and reduced vitamin D activation. The resulting neuromuscular excitability produces muscle cramps, paraesthesia, tetany, and, in severe cases, cardiac arrhythmias and seizures.
Accurate diagnosis and differentiation of these conditions relies on integrated biochemical assessment, including:
PTH levels, to assess parathyroid activity
serum calcium, to determine the direction of calcium imbalance
serum phosphate, which helps distinguish renal and endocrine causes
vitamin D status, to identify contributory deficiency or impaired activation
Interpreting these values together, rather than in isolation, allows clinicians to identify the underlying mechanism driving mineral imbalance and to tailor management appropriately, whether through surgical intervention, vitamin D and calcium replacement, or treatment of underlying renal disease.
Concept Check
How do calcium-sensing receptors regulate PTH secretion?
Why does PTH increase phosphate excretion despite increasing calcium release from bone?
How does PTH activation of vitamin D enhance calcium homeostasis?
What distinguishes primary from secondary hyperparathyroidism?
Why can hypoparathyroidism lead to tetany?