Placental Hormones: Endocrine Regulation of Pregnancy, Fetal Development and Maternal Adaptation
The placenta is a transient yet remarkably complex endocrine organ that plays a central role in supporting pregnancy. Beyond its functions in nutrient and gas exchange, it produces a diverse array of hormones that regulate maternal physiology, fetal development, immune tolerance and the timing of birth. Because the placenta takes over endocrine roles normally carried out by the ovaries and pituitary gland, it ensures that pregnancy proceeds in a hormonally stable environment. These hormones influence nearly every maternal system, cardiovascular, renal, metabolic and immune, demonstrating the placenta’s essential role as an integrated endocrine regulator.
What You Need to Know
The placenta functions as a temporary but highly active endocrine organ that coordinates pregnancy from implantation through to birth. Its hormones act on both maternal and fetal systems, ensuring uterine stability, adequate nutrient supply, immune tolerance and preparation for parturition. Unlike other endocrine organs, placental hormone production changes dynamically across gestation, with different hormones dominating at different stages to meet evolving physiological demands.
Early in pregnancy, placental hormones preserve the uterine environment and maintain progesterone production until the placenta itself becomes the primary steroid source. As pregnancy progresses, endocrine signalling increasingly shifts toward modifying maternal metabolism, cardiovascular function and musculoskeletal flexibility to support rapid fetal growth and prepare for labour and lactation. These hormonal adaptations explain why pregnancy affects nearly every organ system in the mother.
The major placental hormones and their primary roles include:
Human chorionic gonadotropin (hCG), which maintains the corpus luteum and progesterone production in early pregnancy
Progesterone, which stabilises the endometrium, suppresses uterine contractions and supports immune tolerance
Estrogens, which promote uterine growth, increase uteroplacental blood flow and stimulate breast development
Human placental lactogen (hPL), which alters maternal carbohydrate and lipid metabolism to prioritise fetal nutrition
Relaxin, which increases ligamentous flexibility and prepares the cervix and pelvis for labour
These hormones allow the placenta to act as a central regulator of pregnancy, synchronising maternal adaptation with fetal developmental needs. Disruption of placental endocrine function can therefore have profound consequences for implantation success, fetal growth and pregnancy outcomes, highlighting the placenta’s role as both a reproductive and metabolic endocrine organ.
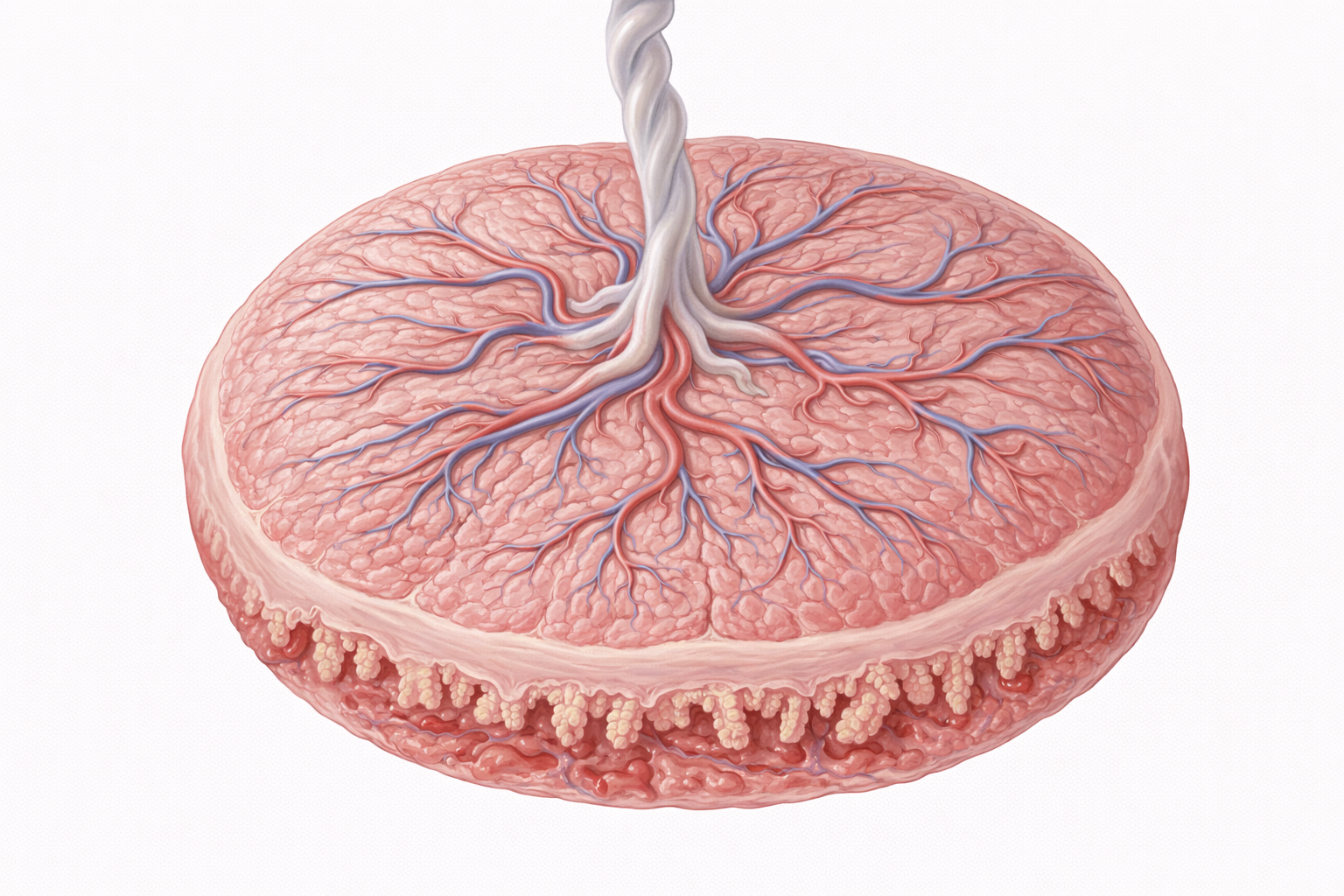
Image: The placenta functions as a temporary endocrine organ, producing hormones that support pregnancy. These include human chorionic gonadotropin (hCG), progesterone, oestrogen, and human placental lactogen (hPL), which act to maintain the uterine environment, regulate maternal physiology, and support fetal development.
Beyond the Basics
Human Chorionic Gonadotropin (hCG)
hCG is the earliest placental hormone, produced by syncytiotrophoblasts shortly after implantation. Its primary role is to rescue and maintain the corpus luteum, ensuring continued progesterone secretion during the first trimester before the placenta is capable of autonomous steroid production. This function is critical for sustaining the endometrium and preventing early pregnancy loss.
As placental steroidogenesis becomes established, hCG levels gradually decline, though low-level secretion persists throughout pregnancy. Clinically, hCG forms the basis of pregnancy testing, and abnormal patterns of rise or decline provide important diagnostic clues. Inappropriately low hCG may indicate ectopic pregnancy or impending miscarriage, while excessively high levels are associated with multiple gestations or gestational trophoblastic disease.
Progesterone: Maintaining Pregnancy
Progesterone is initially produced by the corpus luteum under hCG stimulation and later by the placenta, which becomes the dominant source by the end of the first trimester. Its central role is to maintain uterine quiescence by reducing myometrial excitability and suppressing spontaneous contractions, thereby preventing premature labour.
In addition to its effects on smooth muscle, progesterone thickens cervical mucus to create a barrier against ascending infection and contributes to maternal immune tolerance of the fetus by modulating inflammatory and immune pathways. It also promotes lobuloalveolar development of breast tissue in preparation for lactation, though high progesterone levels suppress milk secretion until after delivery.
Estrogens: Growth, Vascular Adaptation and Parturition
Placental estrogens, particularly estriol, are synthesised through cooperation between the placenta and fetal adrenal glands, making their production a marker of fetoplacental unit function. Estrogens stimulate uterine enlargement, increase uteroplacental blood flow and support breast ductal development, facilitating the structural adaptations required for pregnancy.
As term approaches, rising estrogen levels shift the hormonal balance within the uterus. Estrogens increase myometrial sensitivity to oxytocin and promote prostaglandin synthesis, contributing to cervical ripening and the coordinated contractile activity required for labour.
Human Placental Lactogen (hPL): Metabolic Reprogramming
hPL is produced in large quantities by the syncytiotrophoblast and plays a major role in altering maternal metabolism to support fetal growth. It induces a state of physiological insulin resistance, reducing maternal glucose uptake and ensuring a steady supply of glucose to the fetus. Simultaneously, it promotes lipolysis, increasing the availability of free fatty acids for maternal energy use.
While these changes are adaptive, excessive hPL-mediated insulin resistance can contribute to gestational diabetes in susceptible individuals. hPL also supports breast development and may contribute to lactation readiness, although its precise role in postpartum milk production remains less clearly defined.
Relaxin: Softening and Adaptation of Maternal Tissues
Relaxin is secreted by both the corpus luteum and the placenta and contributes to structural adaptation of maternal tissues. It increases ligamentous laxity, facilitates pelvic expansion and promotes cervical softening, all of which support the mechanical demands of labour and delivery.
Beyond its musculoskeletal effects, relaxin increases renal blood flow and glomerular filtration rate during pregnancy. This supports expanded plasma volume and enhances clearance of metabolic waste for both the mother and fetus, illustrating its broader role in systemic physiological adaptation.
Placental CRH and Endocrine Timing of Birth
The placenta produces corticotropin-releasing hormone (CRH), with circulating levels rising progressively throughout pregnancy and peaking near term. Unlike hypothalamic CRH, placental CRH is stimulated rather than suppressed by cortisol, creating a positive feedback loop between the placenta and fetal adrenal glands.
Placental CRH accelerates fetal adrenal cortisol production, promoting lung maturation and surfactant synthesis. Rising CRH levels also enhance myometrial contractility and prostaglandin production, contributing to the endocrine cascade that governs the timing of parturition.
Immunomodulatory and Paracrine Signals
In addition to classical endocrine hormones, the placenta secretes cytokines, growth factors and locally acting proteins that regulate maternal immune tolerance. These signals suppress rejection of the genetically distinct fetus while preserving the mother’s ability to respond to infection.
This finely balanced paracrine and endocrine environment is essential for maintaining pregnancy. Disruption of these immunomodulatory signals is implicated in complications such as pre-eclampsia, recurrent miscarriage and fetal growth restriction, highlighting the placenta’s role as both an endocrine and immunological interface.
Clinical Connections
Placental endocrine dysfunction produces recognisable patterns of pregnancy complication because placental hormones regulate uterine stability, maternal metabolism and fetal growth simultaneously. When placental hormone output is inadequate or excessive, clinical consequences often emerge before structural abnormalities are evident on imaging, making endocrine interpretation central to obstetric assessment and risk stratification.
Reduced progesterone support compromises uterine quiescence and endometrial stability, increasing the risk of early pregnancy loss and preterm labour. Excessive human placental lactogen activity exaggerates pregnancy-related insulin resistance, tipping susceptible individuals into gestational diabetes. Abnormal trajectories of estrogen or hCG may reflect impaired placental development, fetal compromise or trophoblastic pathology rather than isolated maternal endocrine disease.
Common complications linked to placental endocrine disturbance include:
Miscarriage and preterm labour associated with inadequate progesterone support
Gestational diabetes driven by excessive hPL-mediated insulin resistance
Placental insufficiency or trophoblastic disease suggested by abnormal hCG or estrogen levels
Preterm birth and fetal growth restriction linked to dysregulated placental CRH signalling
Placental CRH plays a particularly important role in the timing of birth, and abnormal elevation earlier in pregnancy is associated with premature activation of labour pathways. Conversely, insufficient endocrine signalling from the placenta can impair fetal adrenal maturation and growth, contributing to low birth weight and neonatal complications.
Concept Check
How does hCG ensure pregnancy maintenance during the first trimester
Why is progesterone essential for preventing premature uterine activity
How does hPL alter maternal metabolism to prioritise fetal growth
What physiological adaptations are driven by rising estrogen levels in pregnancy
How does placental CRH influence fetal development and the timing of labour