Hair and Hair Follicle Anatomy, Structure & Growth Cycle
Hair is a specialised keratinous structure that emerges from deeply embedded follicles within the skin. Although often associated with appearance, its biological roles include protection, sensory perception, thermal insulation and the dispersal of secretions such as sebum. Each hair shaft is supported by a complex follicular unit composed of epithelial and connective tissue elements that coordinate growth, pigmentation and cycling. Understanding the anatomy of the hair and follicle provides insight into conditions such as alopecia, folliculitis and hormonal hair pattern changes, as well as the mechanisms underlying hair growth and regeneration.
What You Need to Know
Hair follicles are specialised epidermal structures that extend deep into the dermis and, in some regions, into the hypodermis. Each follicle functions as a highly organised mini-organ responsible for producing the hair shaft and regulating its growth, pigmentation and cycling. Although the visible hair shaft is composed of dead, keratinised cells, the follicle itself is metabolically active and relies on continuous interaction between epithelial cells and underlying mesenchymal tissue.
Key structural and functional components of the hair follicle include:
The dermal papilla, which provides vascular supply and growth signals to the follicle
Matrix cells, which rapidly divide to form the hair shaft and inner root sheath
The inner and outer root sheaths, which support, shape and anchor the growing hair
Associated structures such as sebaceous glands and the arrector pili muscle, which contribute to lubrication, thermoregulation and sensory responses
Hair growth is cyclical rather than continuous. During the anagen phase, matrix cells proliferate rapidly, producing the hair shaft. This is followed by catagen, a brief involution phase marked by controlled apoptosis and follicle regression. The telogen phase represents a resting period, after which the cycle recommences. These stages are tightly regulated by local signalling pathways involving growth factors, hormones and immune mediators. Proper coordination of follicular structure and cycling is essential not only for hair production but also for skin integrity, sensation and thermoregulation.
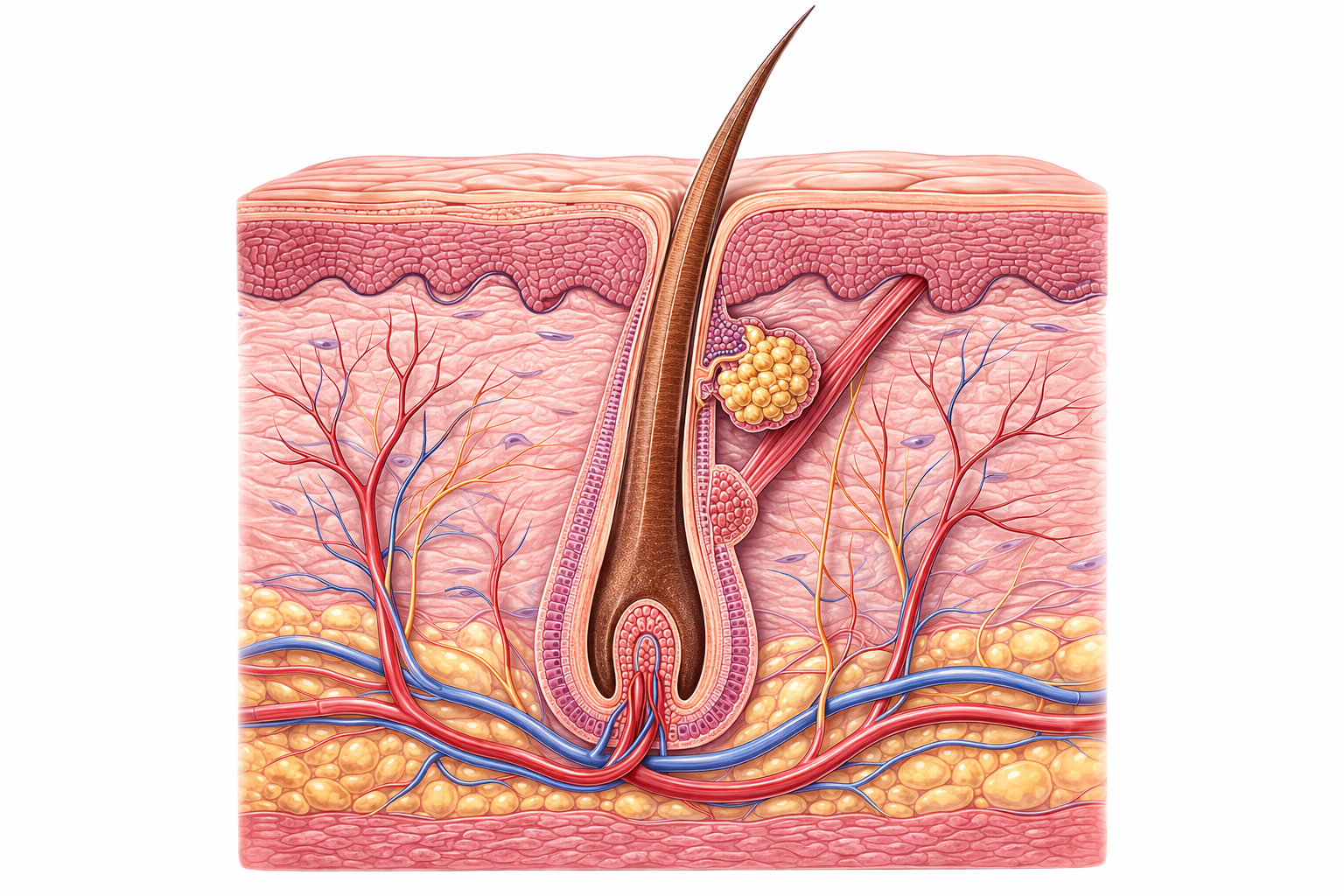
Image: The hair follicle is a specialised skin structure that produces and anchors the hair shaft. At its base, the dermal papilla supplies blood to rapidly dividing matrix cells, which generate the hair and its surrounding root sheaths. Associated structures, including the sebaceous gland and arrector pili muscle, support lubrication and hair movement within the skin.
Beyond the Basics
Structure of the hair shaft
The visible hair shaft is composed of tightly packed, fully keratinised cells organised into three concentric layers. The central medulla, which is present mainly in thicker terminal hairs, contains loosely arranged cells and air-filled spaces that may contribute to insulation and structural bulk. Surrounding this is the cortex, the thickest and most functionally important layer. The cortex contains densely packed keratin macrofibrils and melanin granules, which together determine the hair’s tensile strength, elasticity and colour.
Encasing the cortex is the cuticle, formed by overlapping, flattened cells arranged like roof tiles. This outer layer protects the internal structure of the hair shaft and plays a key role in surface smoothness, light reflection and resistance to physical and chemical damage. Variations in hair thickness, curl pattern and mechanical strength arise from differences in follicle shape, keratin composition and the internal organisation of cortical cells rather than from differences in the hair shaft alone.
The hair follicle as a specialised mini-organ
The hair follicle is a complex, self-renewing structure that functions as a mini-organ within the skin. At its base lies the hair bulb, which surrounds the dermal papilla. The dermal papilla is a specialised cluster of fibroblasts supplied by a rich capillary network and acts as the key signalling centre that regulates hair growth, size and cycling. Growth factors and molecular cues released from the dermal papilla directly influence the behaviour of adjacent matrix cells.
Matrix cells are among the most rapidly dividing cells in the body. They proliferate and differentiate to form the hair shaft and the inner root sheath, which moulds and supports the growing hair as it ascends through the follicle. The inner root sheath disintegrates near the level of the sebaceous duct, allowing the hair shaft to emerge freely. The outer root sheath, a downward extension of the epidermis, provides structural support and houses epithelial stem cells that are essential for follicular regeneration and contribute to epidermal repair following skin injury.
Pigmentation and melanocyte activity within the follicle
Melanocytes located in the hair bulb are responsible for hair pigmentation. Unlike epidermal melanocytes, follicular melanocytes deliver melanin directly into the keratinocytes forming the cortex of the hair shaft. The type, amount and distribution of eumelanin and pheomelanin determine hair colour. During ageing, melanocyte activity within the follicle gradually declines, leading to reduced melanin transfer and the appearance of grey or white hair.
Disruption of melanocyte function within the follicle produces distinctive clinical patterns. Localised loss of pigmentation results in poliosis, while more generalised decline contributes to age-related greying. These changes reflect altered melanocyte activity rather than changes in hair shaft structure.
Sebaceous glands and arrector pili muscles
Most hair follicles are associated with sebaceous glands, which secrete sebum into the follicular canal. Sebum lubricates both the hair shaft and surrounding skin, supports barrier function and exerts antimicrobial effects. Sebaceous activity is hormonally regulated, particularly by androgens, explaining changes in sebum production across the lifespan and in endocrine disorders.
The arrector pili muscle is a small bundle of smooth muscle that connects the follicle to the surrounding dermis. When it contracts in response to cold or emotional stimuli, the hair shaft is elevated, producing goosebumps. While this response has minimal thermoregulatory value in humans, it reflects an evolutionary mechanism for insulation and threat display that remains neurologically intact.
The hair growth cycle and follicular dynamics
Hair growth occurs in a repeating cycle regulated by coordinated signalling between follicular stem cells, matrix cells and the dermal papilla. The anagen phase is the active growth stage, during which matrix cells proliferate continuously and produce the hair shaft. The duration of anagen varies widely depending on body region and determines maximum hair length.
Catagen is a brief involution phase characterised by controlled apoptosis of the lower follicle and separation from the dermal papilla. This is followed by telogen, a resting phase in which the follicle remains metabolically quiet before re-entering anagen. As a new anagen phase begins, the emerging hair eventually displaces the old shaft. Disruption of this tightly regulated cycle by hormonal changes, stress, immune activity or nutritional deficiency leads to altered hair density and shedding patterns, such as androgenic alopecia or telogen effluvium.
Integration with surrounding skin structures
Hair follicles are richly innervated and play an important sensory role. Movement of the hair shaft stimulates surrounding nerve endings, enhancing detection of light touch and environmental changes. The follicle’s close association with sebaceous glands, arrector pili muscles, immune cells and the dermal vascular network highlights its integration within the broader skin environment.
Because of this interconnectedness, systemic illness, endocrine imbalance and inflammatory skin disease often manifest through changes in hair growth, texture or distribution. The hair follicle therefore serves not only as a site of hair production but also as a sensitive indicator of wider physiological and pathological processes within the body.
Clinical Connections
Hair and follicle disorders arise when normal regulation of follicular growth, immune privilege or structural integrity is disrupted. Because the hair follicle is a highly active, immune-sensitive mini-organ, even subtle systemic or local changes can produce visible alterations in hair density, distribution or texture.
In clinical practice, follicular dysfunction most commonly presents as:
Altered growth cycling leading to hair thinning, shedding or loss
Immune-mediated damage targeting the follicular bulb or stem cell niche
Structural or infectious involvement of the follicle and surrounding skin
Alopecia areata results from autoimmune attack on the hair follicle, particularly the bulb region during anagen, leading to sudden, well-defined patches of hair loss. Androgenic alopecia reflects genetically determined sensitivity of scalp follicles to androgens, causing progressive miniaturisation of the follicle and shortening of the anagen phase. Inflammatory or infectious processes such as folliculitis arise when follicular openings become occluded or traumatised, commonly in areas of friction, shaving or moisture retention.
Systemic therapies and hormonal states also have predictable effects on hair. Chemotherapy-induced alopecia occurs because cytotoxic agents preferentially damage rapidly dividing matrix cells, abruptly halting anagen growth. In contrast, hypertrichosis or hirsutism may develop in response to endocrine imbalance or medication effects, reflecting prolonged anagen activity or androgen stimulation of follicles. Understanding follicular anatomy and physiology enables clinicians to interpret these patterns, anticipate reversible versus permanent changes, and guide patient education and management.
Concept Check
How do matrix cells and the dermal papilla work together to support hair growth?
Why does hair colour decline with age?
What structural differences in the follicle contribute to variations in hair texture and curl pattern?
How does the hair growth cycle explain conditions such as telogen effluvium?
Why is the outer root sheath important in both hair regeneration and wound healing?