The Integumentary System - Overview
The integumentary system is the body’s largest and most visible system, forming a multilayered protective barrier that separates the internal environment from the external world. It consists of the skin, hair, nails, sweat glands, sebaceous glands, and numerous sensory receptors. More than just a physical covering, the integumentary system plays essential roles in temperature regulation, fluid balance, immune defence, sensory perception, and the synthesis of vitamin D. The skin itself is highly active, constantly renewing, responding to injury, and interacting with the nervous, circulatory, and immune systems.
What You Need to Know
The integumentary system is the body’s largest organ system and serves as a multifunctional interface between the internal environment and the outside world. It includes the skin and its appendages: hair, nails, sweat glands and sebaceous glands. Together, these structures provide protection, sensory input, temperature regulation, immune defence and metabolic support. Far from being a passive covering, the integumentary system is metabolically active, highly vascular and tightly integrated with the nervous, immune and endocrine systems.
The skin itself is organised into distinct layers that work together to maintain homeostasis. The epidermis provides a resilient barrier and immune surveillance, the dermis supplies structural strength, elasticity and vascular support, and the hypodermis contributes insulation, energy storage and shock absorption. Continuous cellular turnover, repair mechanisms and adaptive responses allow the system to respond dynamically to injury, environmental stress and physiological change.
Key functions of the integumentary system include:
Barrier protection, preventing excessive water loss and blocking pathogens, chemicals and physical injury
Thermoregulation, through cutaneous blood flow, sweating and insulation
Sensory perception, via specialised receptors for touch, pressure, temperature and pain
Immune defence, including innate and adaptive immune activity within the skin
Metabolic roles, such as vitamin D synthesis and lipid storage
Communication and identity, through pigmentation, hair distribution and scent
These functions are interdependent. For example, barrier disruption alters immune responses, thermoregulation affects wound healing, and pigmentation influences UV protection and cancer risk. Changes in skin appearance often provide early clues to systemic illness, nutritional deficiencies, endocrine disorders or immune dysfunction.
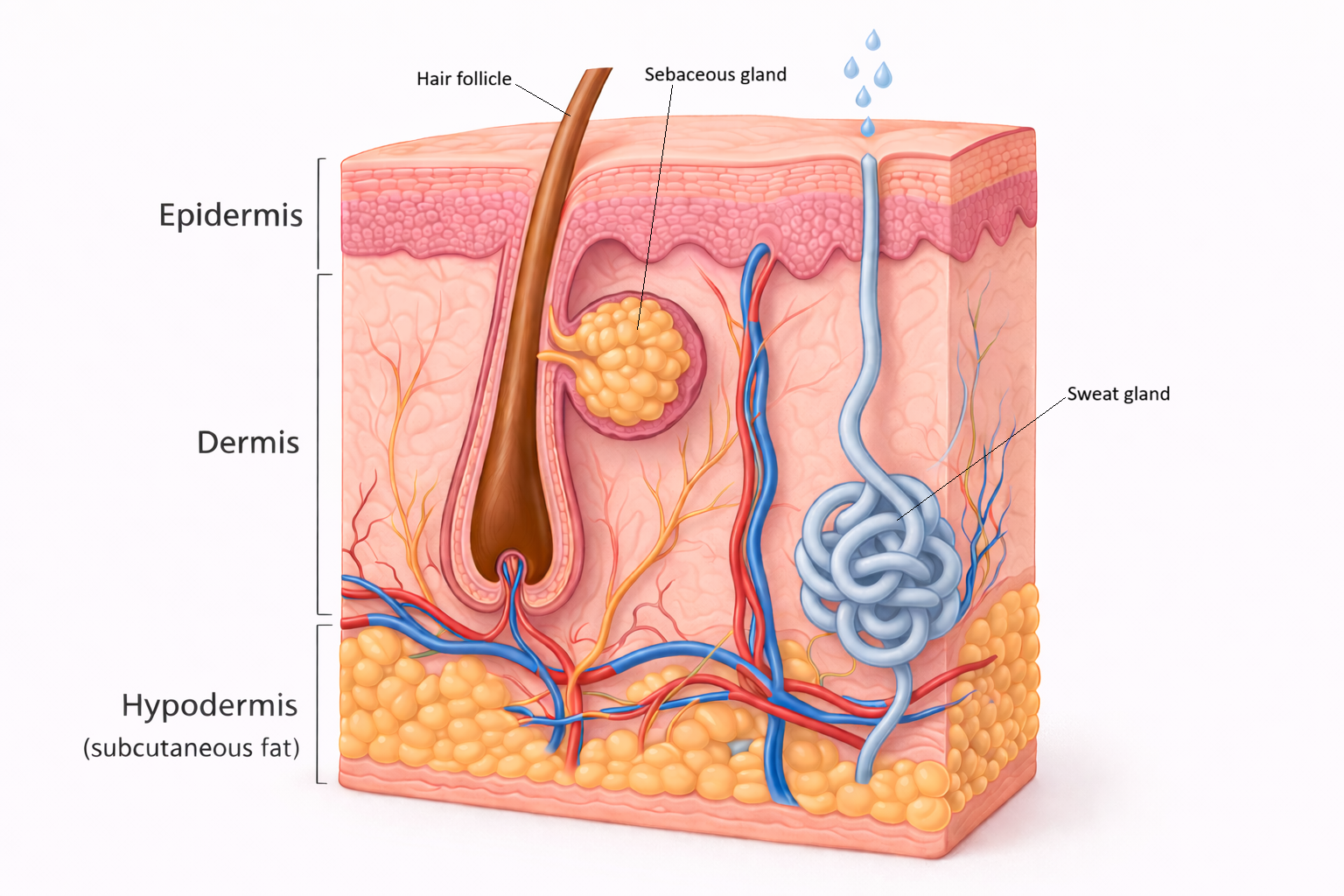
Image: Layers and structures of the skin.
Beyond the Basics
The Integumentary System and Immune Integration
The integumentary system functions as an active immune organ rather than a passive physical barrier. Keratinocytes, which make up the majority of epidermal cells, respond rapidly to injury, infection and ultraviolet exposure by releasing cytokines and chemokines. These signalling molecules attract immune cells, regulate inflammation and help coordinate local defence responses. In this way, keratinocytes act as early warning sensors that translate environmental threats into immune activity.
Embedded within the epidermis are Langerhans cells, specialised antigen-presenting cells that sample microbes and damaged proteins at the skin surface. Once activated, they migrate to regional lymph nodes and initiate adaptive immune responses by activating T lymphocytes. This ability to link local skin exposure with systemic immune activation highlights the skin’s role as a frontline immune organ.
Wound Healing as a Coordinated Biological Process
Wound healing is a complex, staged process that restores tissue integrity after injury. It begins with rapid blood clot formation and immune activation to prevent bleeding and limit infection. This is followed by an inflammatory phase, during which immune cells clear debris and release growth factors. Fibroblasts then proliferate and produce collagen, forming granulation tissue that provides structural support. Finally, epithelial cells migrate across the wound surface to re-establish the epidermal barrier, and the tissue undergoes remodelling to regain strength.
This process is highly sensitive to systemic conditions. Adequate nutrition supplies the building blocks for collagen synthesis, oxygenation supports cellular metabolism, and good perfusion ensures delivery of immune cells and nutrients. Elevated blood glucose impairs immune function and collagen formation, while infection prolongs inflammation and disrupts healing. These interdependencies explain why wound outcomes reflect overall physiological health rather than local injury alone.
Thermoregulation and Neural Control
The skin plays a central role in maintaining stable body temperature through coordinated vascular and glandular responses. When core temperature rises, cutaneous blood vessels dilate, increasing blood flow near the skin surface so heat can be lost to the environment. At the same time, eccrine sweat glands secrete sweat, which cools the body as it evaporates. When temperature falls, vasoconstriction reduces blood flow to the skin, conserving heat and preserving core temperature.
These responses are controlled by neural pathways coordinated by the hypothalamus. Disruption of skin blood flow or sweating, as occurs in burns, severe infection or neurological disease, can destabilise body temperature rapidly. Because temperature regulation is closely tied to cardiovascular and neurological function, failure of these mechanisms can quickly become life-threatening.
Vitamin D Synthesis and Systemic Effects
The integumentary system also contributes to metabolic health through vitamin D synthesis. When ultraviolet B radiation reaches the skin, it converts a cholesterol-derived molecule in the epidermis into a vitamin D precursor. This compound is then transported to the liver and kidneys, where it is converted into its active hormonal form. Active vitamin D plays a critical role in calcium absorption, bone mineralisation and neuromuscular function.
Several factors influence this pathway. Reduced sun exposure, increased skin pigmentation, extensive clothing coverage and sunscreen use all decrease ultraviolet penetration and limit vitamin D production. As a result, deficiency can develop even in sun-rich environments. This illustrates how skin function is tightly linked to skeletal health, immune regulation and long-term metabolic balance.
An Integrated Organ System
Taken together, these processes demonstrate that the integumentary system operates as a highly integrated organ system. Immune defence, wound repair, temperature regulation and metabolic activity are not separate functions but overlapping roles that depend on intact skin structure and signalling. Changes observed at the skin surface often reflect deeper physiological processes, reinforcing the importance of understanding skin function within the broader context of whole-body homeostasis.
Clinical Connections
Assessment of the integumentary system provides valuable insight into overall physiological status because the skin reflects changes in circulation, hydration, immune activity and metabolic function. Alterations in colour, temperature, turgor, moisture, texture or the presence of lesions often appear early and may signal systemic disease before laboratory abnormalities develop.
Common clinically relevant skin findings include:
Colour changes such as pallor, cyanosis or jaundice, which may indicate anaemia, hypoxia or liver dysfunction
Temperature and moisture changes, where cool or clammy skin suggests shock or poor perfusion, and excessive dryness or sweating reflects autonomic or metabolic disturbance
Altered turgor and texture, often associated with dehydration, ageing or connective tissue disease
Lesions or rashes, which may represent infection, allergic reactions, autoimmune disease or medication effects
Pressure injuries remain a major clinical concern, particularly in individuals who are immobile, critically ill or neurologically impaired. Prolonged pressure, friction and shear compromise capillary blood flow, leading to tissue ischaemia and necrosis. Because early skin changes may be subtle, routine inspection and risk assessment are essential for prevention rather than reactive treatment.
Severe integumentary injury, such as burns, disrupts multiple homeostatic functions simultaneously. Loss of the skin barrier leads to rapid fluid shifts, impaired thermoregulation and heightened infection risk. The depth and total body surface area involved determine the severity of systemic consequences, including shock, metabolic stress and long-term functional impairment.
Chronic inflammatory skin conditions such as dermatitis, psoriasis and eczema involve persistent immune activation and barrier dysfunction. These conditions can significantly affect quality of life through pain, pruritus, sleep disturbance and secondary infection. Infectious skin disorders, including cellulitis, fungal infections and viral lesions, require early recognition to prevent local spread or systemic involvement.
Many systemic diseases manifest clearly through the skin. Diabetes is associated with impaired wound healing, neuropathy-related injuries and increased susceptibility to infection. Liver disease may present with jaundice and pruritus, while heart failure often causes peripheral oedema. Autoimmune diseases such as lupus produce characteristic rashes that aid diagnosis. Recognising these patterns reinforces the importance of integumentary assessment as a core component of comprehensive clinical evaluation across all care settings.
Concept Check
How do the structural differences between the epidermis and dermis contribute to their unique functions?
Explain how the skin participates in thermoregulation and why these mechanisms can fail in certain conditions.
Describe the processes involved in wound healing and explain how systemic factors can impair successful recovery.
How does the integumentary system support immune defence, and which specialised cells play a role in this function?
A patient presents with jaundice, itching, and pale stools. Which systemic condition might be responsible, and how does the skin reflect this dysfunction?