Sensory Receptors of the Skin: Mechanoreception, Thermoreception and Nociception
The skin is the body’s largest sensory organ, containing an intricate network of specialised receptors that detect touch, pressure, vibration, temperature and pain. These receptors convert mechanical or thermal energy into electrical signals that travel to the central nervous system, allowing the brain to interpret fine details about the external environment.
Sensory receptors differ in structure, depth, adaptation speed and stimulus specificity, enabling the skin to perceive a remarkable range of sensations—from the light brush of air to deep pressure or painful injury. Understanding these receptors is crucial for recognising how the body detects harm, perceives texture, performs precision movements and maintains protective behaviours.
What You Need to Know
The skin is a highly specialised sensory organ that allows the body to detect and interpret mechanical, thermal and potentially harmful stimuli from the external environment. This sensory input is essential for protection, fine motor control, temperature regulation and pain perception. Cutaneous sensory receptors are unevenly distributed across the body and vary in depth, structure and function, enabling detection of both subtle and intense stimuli.
Sensory receptors in the skin can be broadly grouped according to the type of stimulus they detect and how they respond to sustained input. Their location within the skin layers influences what they sense and how quickly they adapt. Superficial receptors are better suited to detecting fine detail and light touch, while deeper receptors respond to stretch, vibration and sustained pressure.
Key functional characteristics of cutaneous sensory receptors include:
Stimulus specificity, meaning each receptor type is tuned to a particular form of mechanical, thermal or noxious input
Receptive field size, which determines how precisely stimulus location can be identified
Adaptation rate, describing how quickly a receptor reduces its firing during a constant stimulus
Depth within the skin, influencing whether the receptor detects surface-level or deeper mechanical changes
Mechanoreceptors detect physical deformation of the skin. Merkel discs respond to light touch and texture, particularly in areas requiring fine discrimination such as fingertips. Meissner corpuscles detect rapid changes in touch and movement across the skin surface. Pacinian corpuscles, located deeper in the dermis and hypodermis, are highly sensitive to vibration and deep pressure. Ruffini endings respond to sustained stretch and contribute to the perception of skin tension and joint position.
Thermoreceptors are free nerve endings that respond to changes in skin temperature. Distinct populations detect warmth and cold, allowing rapid detection of environmental temperature shifts. These receptors also contribute to thermoregulatory reflexes by providing input to the hypothalamus.
Nociceptors respond to stimuli that threaten tissue integrity, including extreme temperatures, mechanical injury and chemical irritation. Activation of nociceptors produces pain, which serves a protective function by promoting withdrawal and avoidance. Some nociceptors respond immediately to sharp injury, while others mediate slower, dull or burning pain, reflecting differences in nerve fibre type and conduction speed.
Together, these receptors form an overlapping sensory network rather than isolated pathways. Information from multiple receptor types is integrated by the nervous system to determine the location, intensity and quality of a stimulus. This layered organisation allows humans to perform delicate tasks, respond rapidly to danger and adapt behaviour based on continuous sensory feedback from the skin.
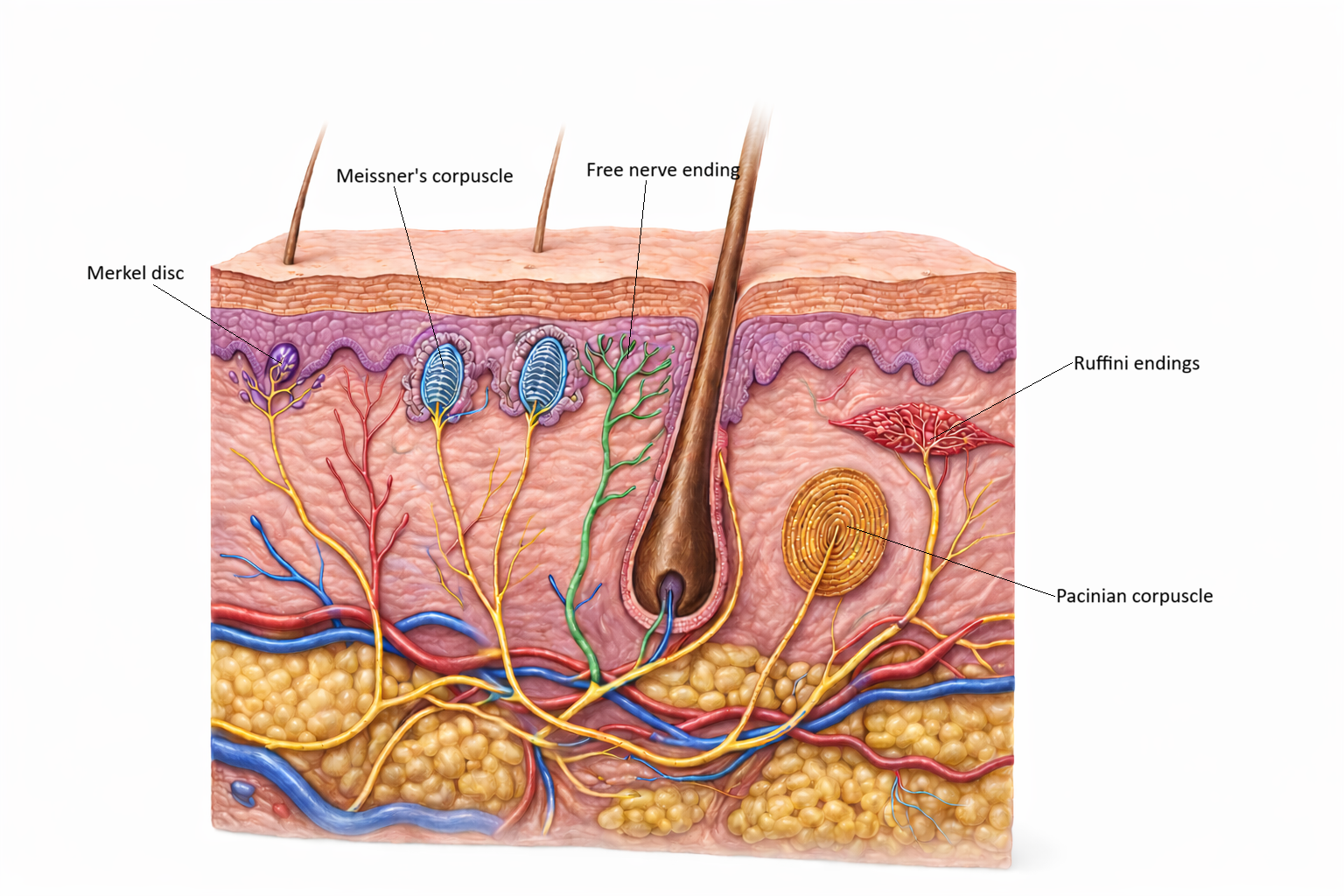
Image: Merkel discs, located in the basal layer of the epidermis, detect light touch and texture. Meissner’s corpuscles, found in the dermal papillae, respond to light touch and low-frequency vibration. Free nerve endings are widely distributed throughout the epidermis and dermis, detecting pain, temperature, and crude touch. Pacinian corpuscles lie deep in the dermis and hypodermis, sensing deep pressure and high-frequency vibration. Ruffini endings, located in the dermis, respond to skin stretch and sustained pressure.
Beyond the Basics
Merkel Discs: Fine Touch and Texture Discrimination
Merkel discs, also referred to as Merkel cell–neurite complexes, are slow-adapting mechanoreceptors located in the basal layer of the epidermis and around hair follicles. Their small receptive fields allow highly precise spatial resolution, making them particularly sensitive to edges, points and fine textures. Each Merkel cell forms a specialised synapse-like junction with an afferent nerve ending, enabling sustained firing during continuous pressure. This persistent signalling is essential for tasks requiring tactile precision, such as reading Braille, manipulating small objects and assessing surface roughness. Clinically, reductions in Merkel receptor density contribute to diminished tactile discrimination in ageing and in peripheral neuropathies.
Meissner Corpuscles: Light Touch and Movement Across the Skin
Meissner corpuscles are rapidly adapting mechanoreceptors located within the dermal papillae of glabrous skin, including the fingertips, palms and lips. Encapsulated within layers of connective tissue, they are optimised to detect low-frequency vibration and light, dynamic touch. Their rapid adaptation means they respond strongly to changes in stimulation rather than sustained pressure. This property is critical for detecting slip and enabling fine adjustments in grip force during object manipulation. Damage to Meissner corpuscles, such as in diabetic neuropathy or peripheral nerve injury, reduces sensitivity to light touch and compromises fine motor control.
Pacinian Corpuscles: Deep Vibration and High-Frequency Pressure
Pacinian corpuscles are located deep within the dermis and hypodermis and are among the largest sensory receptors in the body. Their distinctive onion-like lamellar structure surrounds a central nerve ending that is exquisitely sensitive to mechanical deformation. These receptors respond preferentially to high-frequency vibration and deep pressure and adapt very rapidly, firing mainly at the onset and offset of stimulation. Functionally, Pacinian corpuscles allow detection of vibrations transmitted through objects, such as those experienced when writing with a pen, typing on a keyboard or handling tools and machinery.
Ruffini Endings: Skin Stretch and Finger Position
Ruffini endings are slow-adapting mechanoreceptors found in the deep dermis. They respond to sustained skin stretch rather than discrete pressure points, providing information about overall tension and deformation patterns. Their broad receptive fields make them particularly important for proprioceptive feedback, grip modulation and hand positioning. In the fingers, Ruffini endings contribute to coordinated movement and to the perception of object shape during manipulation.
Free Nerve Endings: Pain, Temperature and Itch
Free nerve endings are the most abundant sensory receptors in the skin and extend widely throughout both the epidermis and dermis. Unlike encapsulated mechanoreceptors, they lack specialised structural coverings and instead respond directly to chemical, thermal and mechanical stimuli.
Nociceptors respond to potentially damaging inputs such as extreme temperatures, excessive mechanical force or chemical irritation. Activation of nociceptors produces pain, which serves a protective function by promoting withdrawal and avoidance. Two primary fibre types are involved: A-delta fibres transmit sharp, fast pain, while C fibres transmit slower, dull, aching or burning pain. Sensitisation of nociceptors is a key mechanism in inflammation and chronic pain states.
Thermoreceptors detect changes in temperature rather than absolute temperature values. Separate populations respond to warmth and cold, each with distinct activation thresholds. When temperatures exceed safe limits, thermoreceptor activity overlaps with nociceptor activation, signalling potential tissue injury.
Pruriceptors are specialised free nerve endings, primarily C fibres, that respond to itch-inducing chemical mediators such as histamine. Activation of these receptors triggers scratching behaviours that help remove irritants or parasites but can also exacerbate skin damage when excessive.
Together, free nerve endings provide rapid detection of harmful or potentially harmful stimuli and initiate protective reflexes.
Integration of Sensory Information
Cutaneous sensory receptors function as an integrated network rather than as isolated units. Grasping an object simultaneously engages Merkel discs, Meissner corpuscles and Ruffini endings. Pain perception reflects not only nociceptor activation but also modulation by descending pathways from the central nervous system. Temperature perception depends on receptor type, rate of temperature change and stimulus location. This integration allows the nervous system to construct a nuanced and context-dependent representation of the external environment, supporting fine motor control while maintaining protection from injury.
Clinical Connections
Disruption of cutaneous sensory receptors has significant consequences for safety, mobility and tissue integrity. Conditions such as peripheral neuropathy, burns, spinal cord injury and demyelinating disease alter the transmission or interpretation of sensory input, increasing the risk of unrecognised injury and delayed intervention.
Clinically relevant sensory consequences include:
Loss of mechanoreception, leading to impaired fine motor control, reduced grip stability and increased risk of cuts, pressure injury and repetitive trauma
Nociceptor dysfunction, presenting as reduced pain perception or maladaptive signalling seen in chronic pain syndromes
Impaired thermoreception, predisposing individuals to burns, scalds or frostbite due to failure to detect unsafe temperatures
Reduced pressure sensation, limiting spontaneous repositioning and increasing susceptibility to tissue ischaemia and pressure injuries
Sensory impairment is a key contributor to pressure injury development, particularly in patients who cannot perceive discomfort or sustained pressure. Without protective feedback, prolonged compression of soft tissues compromises perfusion and accelerates skin and deep tissue damage.
Concept Check
Why do Merkel discs play a central role in texture discrimination?
How do Meissner corpuscles contribute to grip control during fine motor tasks?
What structural features allow Pacinian corpuscles to detect high-frequency vibration?
How do Ruffini endings assist with proprioception and hand positioning?
Why do thermoreceptors respond to temperature change rather than absolute temperature?
How does damage to free nerve endings affect protective behaviours?