Sweat & Sebaceous Glands
Sweat glands and sebaceous glands are integral components of the integumentary system, contributing to thermoregulation, barrier protection, hydration and microbial defence. Although often discussed in relation to sweat production or acne, these glands perform highly specialised and tightly regulated physiological functions. Their secretions help maintain the acid mantle, influence the skin microbiome, and play a central role in fluid and electrolyte balance. Understanding how these glands function provides essential insight into bodily temperature control, hydration, odour formation, lubrication and overall skin homeostasis.
What You Need to Know
Sweat and sebaceous glands are specialised skin appendages that play essential roles in thermoregulation, hydration, barrier integrity, and antimicrobial defence. Although small in size, their secretions significantly influence skin health and the body’s ability to respond to environmental and physiological stress. Gland activity is tightly regulated by autonomic innervation, hormonal signals, and local skin conditions.
The major cutaneous glands differ in structure, distribution, and function:
Eccrine sweat glands produce a watery, electrolyte-rich secretion for cooling and hydration
Apocrine sweat glands release a thicker secretion that contributes to body odour after bacterial metabolism
Sebaceous glands secrete lipid-rich sebum that lubricates and protects the skin surface
Eccrine glands are widely distributed across the body and are particularly dense on the palms, soles, and forehead. Their secretion supports evaporative cooling and helps maintain skin hydration. Apocrine glands are concentrated in areas such as the axillae and groin and become active after puberty, responding primarily to emotional and hormonal stimuli rather than temperature alone. Sebaceous glands are closely associated with hair follicles and release sebum, which reduces transepidermal water loss, supports the skin barrier, and inhibits microbial overgrowth. Together, these glands contribute to maintaining a stable skin environment and enable the integumentary system to adapt to changing internal and external demands.
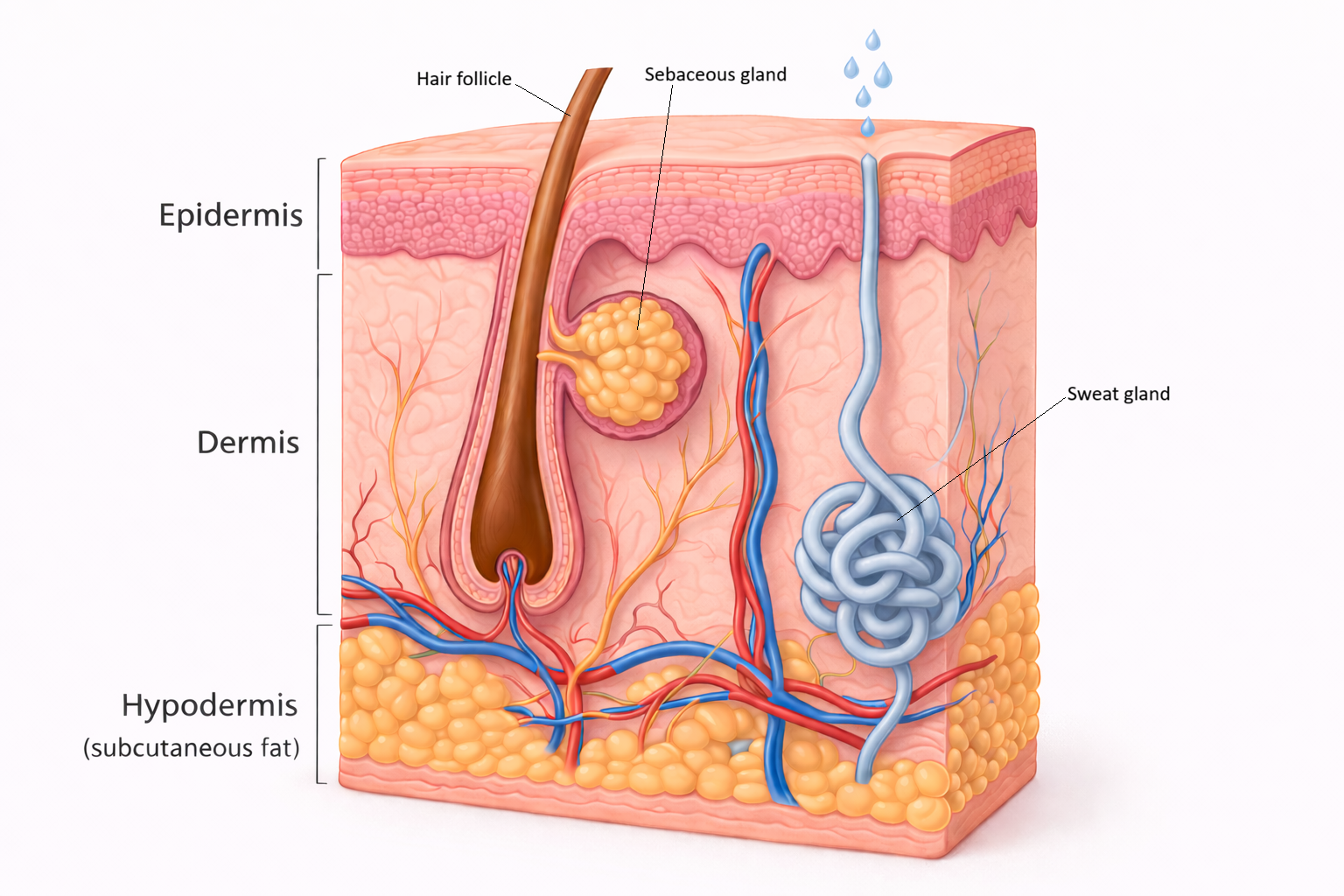
Image: Sebaceous glands secrete sebum into hair follicles to lubricate the skin and hair, while sweat glands produce sweat that is released onto the skin surface for thermoregulation.
Beyond the Basics
Eccrine sweat glands and thermoregulation
Eccrine sweat glands are the most numerous glandular structures in the skin, with millions distributed across the body surface. They are particularly concentrated on the palms, soles, forehead, and trunk. Each eccrine gland consists of a coiled secretory unit located deep within the dermis and a duct that opens directly onto the skin surface. This structural arrangement allows rapid delivery of sweat to the epidermis in response to thermal or emotional stimuli.
The fluid produced by eccrine glands is hypotonic and composed primarily of water, with dissolved electrolytes including sodium, chloride, potassium, lactate, and urea. As sweat passes through the duct, sodium and chloride are reabsorbed, making the final secretion more dilute than plasma. During periods of high sweat output, reabsorption becomes less efficient, leading to greater electrolyte loss. This mechanism explains why prolonged exertion or heat exposure can result in significant sodium depletion if fluids are not adequately replaced.
Eccrine glands are innervated by sympathetic cholinergic fibres, which is unusual given that most sympathetic pathways use adrenergic neurotransmission. Activation increases during heat stress, physical activity, and emotional arousal. Their primary function is evaporative cooling, as heat is absorbed when sweat evaporates from the skin surface. This process is essential for maintaining core temperature, and without eccrine sweat glands, effective thermoregulation in warm environments would not be possible.
Apocrine sweat glands and scent production
Apocrine sweat glands develop at puberty and are found mainly in the axillae, groin, areolae, and perianal region. Unlike eccrine glands, apocrine glands do not contribute significantly to thermoregulation. They produce a thicker, protein- and lipid-rich secretion that is initially odourless when released onto the skin surface.
Apocrine glands are located deeper in the dermis and typically empty into hair follicles rather than directly onto the skin. Their activity is regulated by adrenergic sympathetic innervation and influenced by hormonal signals, particularly androgens. Body odour arises when apocrine secretions are metabolised by skin bacteria, especially species of Corynebacterium, producing volatile compounds responsible for characteristic scents.
Although the precise function of apocrine glands in humans is not fully understood, they are thought to play a role in social signalling and emotional stress responses. Their activation during anxiety or emotional arousal supports the idea that apocrine secretions may function as chemical signals rather than thermoregulatory fluids.
Sebaceous glands and barrier support
Sebaceous glands are holocrine glands, meaning that entire glandular cells rupture to release their contents. This mechanism distinguishes them from eccrine and apocrine glands and results in continuous delivery of sebum to the skin surface. Sebaceous glands are most abundant on the face, scalp, chest, and upper back and are absent on the palms and soles.
Sebum is a complex mixture of triglycerides, wax esters, squalene, and free fatty acids. These lipids form a hydrophobic layer on the skin surface that reduces transepidermal water loss, maintains epidermal flexibility, and supports barrier integrity. Sebum also contributes to antimicrobial defence by inhibiting the growth of certain bacteria and fungi and by maintaining the acidic pH of the skin surface.
Sebaceous gland activity is strongly influenced by androgens, which explains the marked increase in sebum production during puberty and the association between sebaceous overactivity and acne. With advancing age, sebaceous activity declines, contributing to dryness, scaling, and increased skin fragility.
Interaction with the skin microbiome
Sweat and sebum play a central role in shaping the skin microbiome. Eccrine sweat helps maintain an acidic surface pH and mechanically flushes microbes from the skin. Sebum provides lipid substrates that support the growth of commensal organisms, influencing microbial composition and stability. Apocrine secretions, once metabolised by bacteria, contribute to individual scent profiles and local microbial communities.
This biochemical interaction between glandular secretions and microorganisms supports protective immunity by limiting colonisation by pathogenic species while promoting a stable commensal population. Disruption of this balance can contribute to skin disorders such as acne, intertrigo, and certain forms of dermatitis.
Hydration, electrolytes, and endocrine influence
Sweating is essential for thermoregulation but also has implications for fluid and electrolyte balance. Prolonged or excessive sweating can lead to significant losses of sodium and chloride, particularly in unacclimatised individuals. The hormone aldosterone enhances sodium reabsorption in eccrine sweat ducts, resulting in more dilute sweat during heat acclimation.
This adaptive mechanism reduces electrolyte loss during sustained exposure to heat or physical exertion. It highlights the close integration between the integumentary and endocrine systems in maintaining homeostasis under environmental stress.
Age-related and hormonal variation
Glandular function changes across the lifespan. Eccrine glands are functional from early childhood but show reduced responsiveness with age, contributing to impaired thermoregulation in older adults. Apocrine and sebaceous glands become active at puberty under androgen influence, with sebaceous activity declining later in life.
Hormonal fluctuations during menstruation, pregnancy, and menopause further influence sweat and sebum production. These changes help explain variations in skin hydration, odour, and susceptibility to irritation or infection across different life stages.
Clinical Connections
Disorders of sweat and sebaceous glands affect more than surface appearance, as these glands play key roles in thermoregulation, barrier integrity, and microbial control. When gland function is disrupted, clinical consequences often involve inflammation, infection risk, altered temperature regulation, and changes in skin tolerance to moisture and friction.
In clinical practice, glandular dysfunction most commonly presents in the following patterns:
Obstruction or overactivity of sebaceous glands
Excessive or absent eccrine sweating
Chronic inflammation of apocrine-rich regions
Sebaceous gland dysfunction commonly leads to acne, sebaceous cyst formation, or seborrhoeic dermatitis. Excess sebum production and follicular blockage promote inflammation and bacterial overgrowth, while altered lipid composition can impair barrier function and contribute to scaling and irritation. These conditions highlight the role of sebum in maintaining both mechanical protection and microbial balance.
Abnormalities of eccrine sweat glands directly affect thermoregulation. Hyperhidrosis results in excessive sweating that can cause skin maceration, electrolyte disturbance, and social distress, while anhidrosis limits evaporative cooling and increases the risk of heat-related illness. Both conditions reflect failure of normal autonomic and ductal regulation of sweat production and require careful assessment of hydration, temperature tolerance, and environmental exposure.
Apocrine gland disorders are less common but can be clinically significant. Hidradenitis suppurativa is a chronic inflammatory condition affecting apocrine-rich areas such as the axillae and groin, characterised by painful nodules, abscesses, and sinus tract formation. The condition reflects a combination of follicular occlusion, immune dysregulation, and secondary bacterial involvement, rather than isolated sweat gland overactivity.
Linking glandular structure and regulation to clinical presentation helps explain patterns of inflammation, infection risk, odour formation, and fluid imbalance, and guides more effective prevention and management across a wide range of clinical settings.
Concept Check
How do eccrine sweat glands contribute to thermoregulation, and why are they essential for survival in warm environments?
Why does apocrine sweat produce body odour despite being initially odourless?
How does sebum support the skin barrier and influence the skin microbiome?
Which autonomic pathways control eccrine vs apocrine gland activity, and how do they differ?
How do hormonal changes influence sebaceous gland activity across the lifespan?