Joint Structure & Types: Fibrous, Cartilaginous & Synovial Joints
Joints are the anatomical sites where two or more bones meet, and they are fundamental to movement, stability, and load transfer throughout the body. While bones provide the rigid framework of the skeleton, joints determine how that framework can move, absorb forces, and maintain posture. The structure of a joint directly governs its function: some joints are designed for extreme stability with little movement, while others sacrifice stability to permit a wide range of motion. Understanding joint structure and classification is essential for interpreting normal movement, recognising injury patterns, and understanding the pathophysiology of common joint diseases such as osteoarthritis, rheumatoid arthritis, and ligament injuries.
What You Need to Know
Joints are the points where two or more bones meet, allowing the skeleton to move while maintaining overall stability. They are classified both structurally and functionally, but structural classification is the most clinically useful because it explains how a joint is built and therefore how it behaves under stress, movement, and injury. Based on the type of connective tissue between bones and the presence or absence of a joint cavity, joints are divided into three major categories.
Fibrous joints - Bones are connected by dense fibrous connective tissue with no joint cavity. These joints provide strong, rigid connections and are designed mainly for protection and stability, such as the sutures of the skull.
Cartilaginous joints - Bones are joined by cartilage, allowing limited movement while providing shock absorption and load transfer, as seen in intervertebral discs and the pubic symphysis.
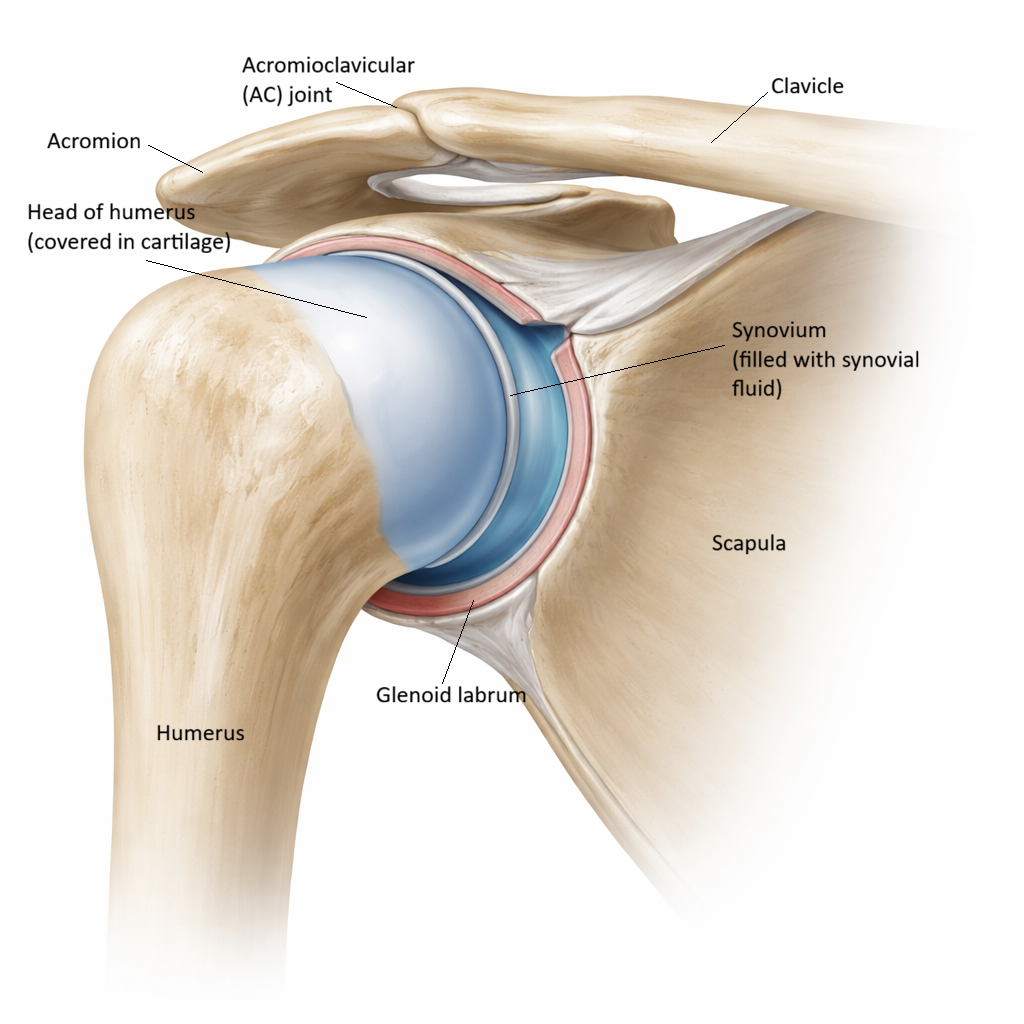
Synovial joints - Bones are separated by a fluid-filled joint cavity and surrounded by a joint capsule, allowing a wide range of motion. These joints are specialised for movement and are found in the limbs, such as the shoulder, hip, knee, and elbow.
This structural organisation determines how much movement a joint allows, how mechanical forces are distributed, and how likely a joint is to be injured or develop degeneration. Fibrous joints prioritise protection, cartilaginous joints balance stability with flexibility, and synovial joints maximise mobility at the cost of increased vulnerability to wear, inflammation, and trauma.
Image: Synovial joint showing the humeral head articulating with the glenoid cavity, with smooth articular cartilage, a fluid-filled synovial cavity, and a surrounding capsule that allows movement while maintaining stability.
Fibrous Joints: Maximum Stability, Minimal Movement
Fibrous joints are characterised by bones that are tightly bound together by dense, collagen-rich connective tissue. This fibrous tissue acts like very strong rope, holding bones together and resisting separation. These joints provide protection, structural integrity, and resistance to movement rather than mobility. There are three main types of fibrous joints: sutures, syndesmoses, and gomphoses.
Sutures are found exclusively in the skull, where the cranial bones interlock like puzzle pieces. In infancy, these sutures are flexible to allow the skull to expand as the brain grows. With age, the connective tissue gradually ossifies and the bones fuse, forming synostoses (bone-to-bone unions) that create a rigid protective case around the brain.
Syndesmoses are fibrous joints in which bones are connected by ligaments or interosseous membranes. A classic example is the distal tibiofibular joint, where the tibia and fibula are held together by strong ligaments. Although movement is minimal, a small amount of flexibility is essential to absorb forces during walking, running, and weight-bearing.
Gomphoses anchor the roots of teeth into the alveolar sockets of the jaw using the periodontal ligament. These joints must withstand very high compressive forces during chewing while still allowing microscopic movement that helps absorb shock and prevent tooth damage.
Fibrous joints therefore prioritise protection and stability, making them ideal for the skull and other regions where movement would be dangerous.
Cartilaginous Joints: Strength With Limited Flexibility
Cartilaginous joints are united by cartilage, which is tougher and more flexible than bone but stronger than fibrous tissue. This allows more movement than fibrous joints but far less than synovial joints. They are designed to provide strength, shock absorption, and limited motion. There are two major types: synchondroses and symphyses.
Synchondroses are joints in which bones are united by hyaline cartilage, a smooth, glassy cartilage that allows growth and some flexibility. The most important examples are the epiphyseal (growth) plates in children, which allow bones to lengthen during development. These joints eventually ossify and disappear in adulthood, leaving a solid bone. Some permanent synchondroses remain where rigid support with slight flexibility is needed.
Symphyses are joints in which bones are joined by fibrocartilage, a tough, fibrous form of cartilage designed to withstand compression and tension. The pubic symphysis and intervertebral discs are key examples. This fibrocartilage acts as a shock absorber, allowing slight movement while supporting heavy loads, which is essential for walking, lifting, and spinal flexibility.
Cartilaginous joints are therefore ideally suited for parts of the skeleton that must bear weight while allowing controlled movement.
Synovial Joints: The Joints of Movement
Synovial joints are the most complex and mobile joints in the body. Nearly all joints that allow free movement, such as the shoulder, hip, knee, and elbow, belong to this category. Their defining feature is the presence of a synovial cavity, a small fluid-filled space that separates the bone surfaces and allows them to move smoothly over one another. Every synovial joint contains several essential components. The ends of the bones are covered with articular cartilage, which reduces friction and absorbs impact. The joint is enclosed by a fibrous capsule that holds the bones together while still allowing movement. Lining the inside of this capsule is the synovial membrane, which produces synovial fluid.
Synovial fluid is a thick, slippery liquid that lubricates the joint and nourishes the articular cartilage. Because cartilage has no blood supply, it depends entirely on this fluid for oxygen, nutrients, and waste removal. This is why movement is important for joint health: compression and release help circulate synovial fluid through the cartilage. Additional structures improve stability and function. Ligaments strengthen the capsule and limit excessive movement. Tendons transmit muscle force across the joint. Bursae reduce friction between moving tissues, and menisci deepen joint surfaces and distribute load, particularly in weight-bearing joints like the knee.
Types of Synovial Joints and Their Movements
Synovial joints are further classified by the shape of their articulating surfaces and the movements they permit. This shape-function relationship explains why different joints move in different ways.
Hinge joints, such as the elbow and knee, allow bending and straightening (flexion and extension).
Pivot joints, such as the atlanto-axial joint in the neck, allow rotation.
Ball-and-socket joints, such as the hip and shoulder, allow movement in all directions, providing the greatest range of motion.
Condyloid (ellipsoid) joints, such as the wrist, allow movement in two planes.
Saddle joints, such as the thumb joint, permit complex movements needed for grip and opposition.
Plane joints allow small sliding movements between flat bone surfaces.
The structure of each synovial joint determines both how it moves and how it is injured. Highly mobile joints such as the shoulder are more prone to dislocation, while weight-bearing joints such as the knee and hip are more vulnerable to degeneration and load-related injury.
Clinical Connections
Joint structure strongly influences both disease patterns and injury risk. Osteoarthritis primarily affects synovial joints, where progressive degeneration of articular cartilage leads to pain, stiffness, crepitus, and reduced range of motion. Because this cartilage is avascular and relies on diffusion from synovial fluid rather than a direct blood supply, its ability to repair after wear or injury is limited. Over time, repeated mechanical stress and poor cartilage nutrition contribute to irreversible joint damage.
Rheumatoid arthritis is an autoimmune disease that targets the synovial membrane, producing chronic inflammation, excessive synovial fluid, and progressive destruction of cartilage and bone. This explains why synovial joints become swollen, warm, and painful, and why deformities develop as the joint capsule and supporting structures are gradually eroded.
Different joint structures are vulnerable to specific types of injury and disease, leading to distinct clinical consequences such as:
Synovial joints: osteoarthritis, rheumatoid arthritis, dislocations
Cartilaginous joints: disc degeneration, spinal stiffness, nerve compression
Ligament injury: joint instability and accelerated degeneration
High-mobility joints: greater risk of dislocation and soft-tissue damage
Ligament injuries, such as anterior cruciate ligament (ACL) tears, disrupt the stabilising structures of synovial joints. Even when bones and cartilage are intact, instability alters load distribution and joint mechanics, accelerating cartilage wear and increasing the risk of early osteoarthritis. Similarly, intervertebral disc degeneration, a disorder of a cartilaginous joint, reduces shock absorption and spinal flexibility while allowing bulging or herniation that can compress spinal nerves and cause pain or weakness.
Joint dislocations occur almost exclusively at synovial joints because their freedom of movement requires less bony constraint. The shoulder is particularly vulnerable because it sacrifices stability for mobility, making it prone to recurrent dislocation and soft-tissue injury.
Understanding joint structure is essential in trauma assessment, orthopaedic care, rehabilitation, and safe patient handling. It guides imaging interpretation, helps predict patterns of injury and degeneration, and informs how joints should be protected, mobilised, or surgically repaired to restore function and prevent long-term disability.
Concept Check
Why do fibrous joints permit little to no movement?
How does fibrocartilage differ functionally from hyaline cartilage in joints?
Why are synovial joints more prone to dislocation than cartilaginous joints?
How does synovial fluid nourish articular cartilage?
Why does osteoarthritis primarily affect synovial joints?