Escalating Patient Care: The Nurse’s Responsibility
Recognising when a patient is deteriorating is only part of safe practice. Acting on that information is just as important. Nurses are often the first to detect subtle changes, which places them in a key position to initiate escalation. Understanding when to escalate, how to do it, and what is expected professionally ensures that concerns are acted on early and clearly.
What you need to know
Escalation of care means recognising when clinical deterioration is occurring and communicating this in a way that leads to timely review or intervention. It is not limited to emergencies. It includes any situation where a patient’s condition is worsening, not improving as expected, or causing concern.
In practice, escalation may involve:
notifying the nurse in charge or team leader
requesting a medical review
initiating a rapid response or MET call
activating emergency protocols such as a code blue
Escalation is guided by both clinical judgement and structured systems such as early warning scores or escalation criteria. These systems provide thresholds, but they do not replace clinical concern. If there are concerns despite observations being within normal limits, seek clarification from a senior clinician to determine whether escalation is required.
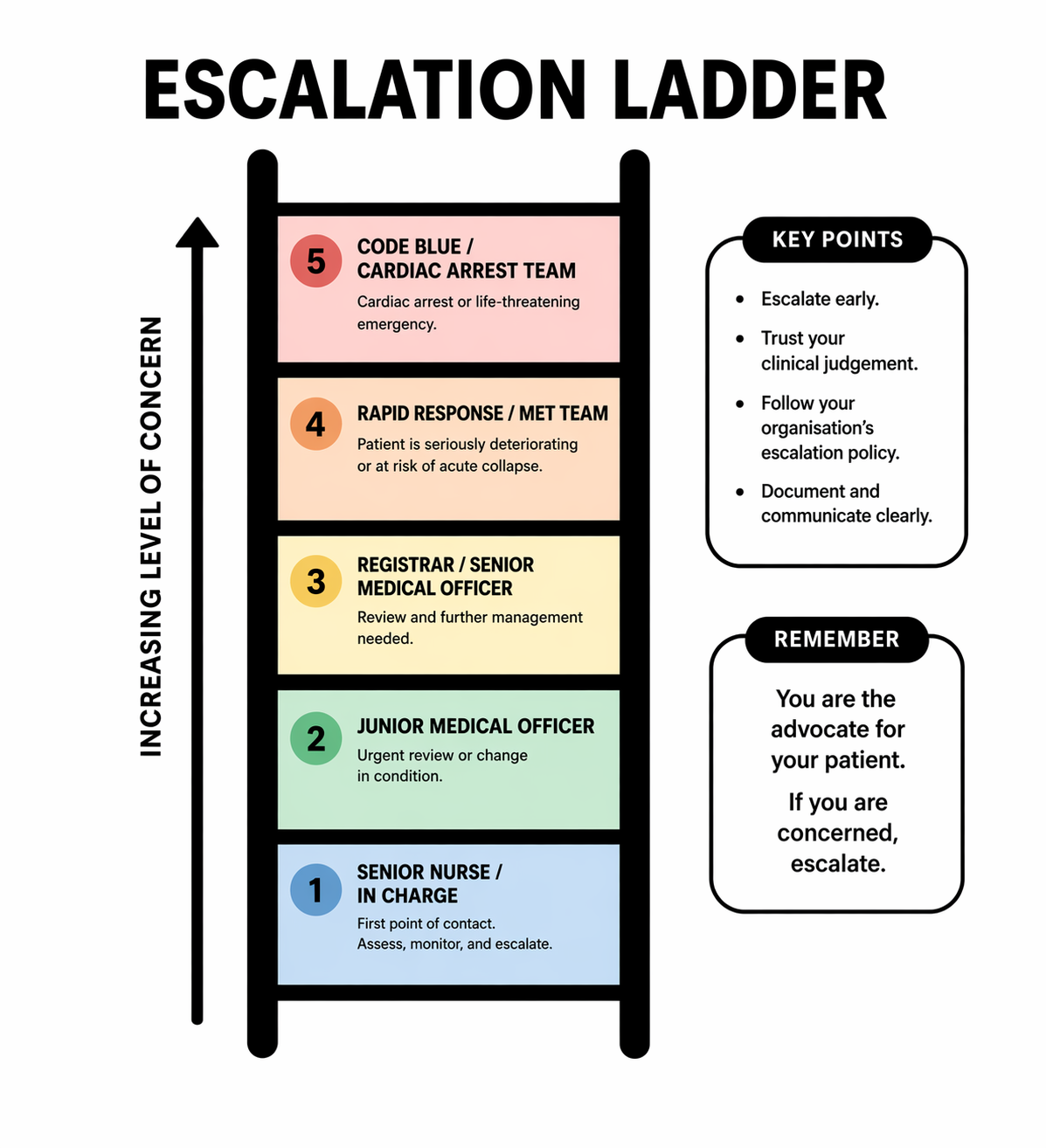
In a clinical setting, there is an escalation ladder, meaning there are different levels of escalation depending on the severity of the patient’s condition and the urgency of the situation. Nurses who are new to the clinical environment may not yet be familiar with the different pathways available, and who to escalate to will depend on how unwell the patient is. Lower-level concerns may be directed to a senior nurse or medical team member, while more serious or rapidly deteriorating patients require urgent escalation through systems such as a MET call or code blue. Understanding this hierarchy ensures concerns are communicated to the right person at the right time.
Beyond the basics
Escalation is not only a clinical task, it is a professional and legal responsibility. Nurses are accountable for recognising deterioration and taking appropriate action. Delays or failure to escalate can lead to preventable harm and may be considered a breach of professional standards and result in disciplinary action.
Clear communication is central to effective escalation. Information should be concise, relevant, and structured. Using tools such as ISOBAR (Identidy, Situation, Observations, Background, Assessment, Recommendations) helps to structure and standardise communication so that key details are not missed. This includes:
identifying the patient
explaining the situation
what the current observations are
providing relevant background
outlining current assessment findings
stating what is needed
Barriers to escalation can occur in practice. These may include uncertainty about clinical findings, lack of confidence, hierarchical dynamics, or previous negative experiences. Despite this, patient safety must take priority. Escalation should not be delayed due to discomfort or fear of being wrong.
Documentation is also part of escalation. This includes recording the patient’s condition, the concern identified, who was notified, the time of escalation, and any actions taken. Accurate documentation provides a clear clinical timeline and supports continuity of care.
In practice
Escalation follows a clear hierarchy, moving from immediate nursing support through to emergency response. Each level has a specific role, and progression depends on the patient’s condition and response to intervention.
A typical escalation hierarchy includes:
the nurse in charge or team leader, for immediate clinical support, review or advice if unsure whether escalation is required
the junior medical officer or intern, for initial medical assessment and management
the registrar or senior medical officer, for more advanced clinical decision-making
the rapid response team or MET call, for acute deterioration requiring urgent intervention
the code blue team, for cardiac or respiratory arrest requiring immediate resuscitation
Escalation should begin at the appropriate level based on the patient’s condition. Mild concerns may start with the nurse in charge, while severe deterioration may require immediate activation of a MET call or code blue without delay. You do not need permission to activate a MET call or code blue. If a patient meets escalation criteria or you are concerned about rapid deterioration, these can be called immediately. Delaying escalation to seek approval can lead to deterioration and is not expected practice.
Each step of escalation requires reassessment. If the patient does not improve, escalation must continue to the next level rather than waiting or assuming the situation will resolve.
Effective use of the escalation hierarchy involves:
identifying the correct starting point based on severity
clearly communicating the concern at each level
reassessing the patient after intervention
escalating further if there is no improvement
Escalation is about ensuring the patient receives timely and appropriate care. Knowing the hierarchy allows nurses to act confidently and avoid delays when a patient’s condition is changing.