Haematologic System - Overview
Haematology is the study of blood, its cellular components, and the organs responsible for producing, regulating, and maintaining it. Blood is a unique connective tissue that circulates through the cardiovascular system, transporting oxygen, nutrients, waste products, hormones, and immune cells to every part of the body. It plays central roles in immunity, thermoregulation, coagulation, and acid–base balance. Because blood interacts with virtually every other body system, haematological disorders can produce wide-ranging effects, from subtle fatigue to life-threatening emergencies.
What You Need to Know
Blood is a specialised connective tissue composed of plasma and formed elements, working together to transport substances, defend the body, and maintain internal stability. Plasma is a clear, straw-coloured fluid that makes up just over half of blood volume and contains water, electrolytes, nutrients, hormones, waste products, clotting factors, and proteins such as albumin and immunoglobulins. It provides the medium for transporting cells and dissolved substances, and changes in plasma composition directly influence blood pressure, fluid balance, and tissue perfusion.
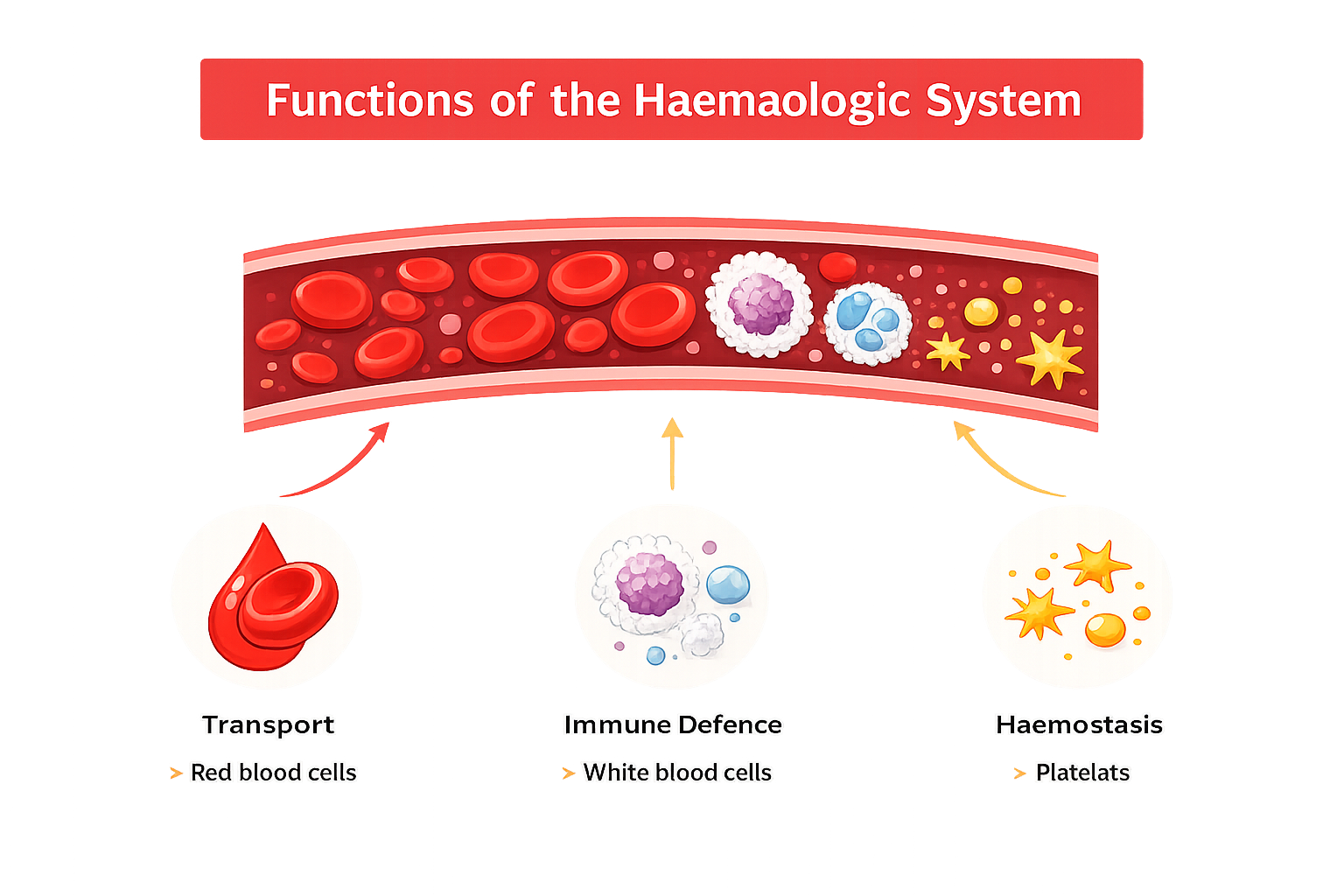
The formed elements consist of three main cell types:
red blood cells, which transport oxygen
white blood cells, which provide immune defence
platelets, which enable clotting
Red blood cells contain haemoglobin, an iron-containing protein that binds oxygen in the lungs and releases it in tissues. The number of red cells, their size, and their haemoglobin content together determine how much oxygen the blood can carry. Disruption of red cell production, haemoglobin synthesis, or cell survival, such as through iron deficiency, chronic disease, or blood loss — reduces oxygen delivery and produces anaemia, leading to fatigue, pallor, breathlessness, and reduced exercise tolerance.
White blood cells circulate between the blood, tissues, and lymphatic system to identify and eliminate infection, damaged cells, and foreign material. Different white cell types perform specialised roles, from rapid bacterial killing to long-term immune memory. Abnormal white cell counts or function may indicate infection, inflammation, immune suppression, or haematological malignancy.
Platelets are small cell fragments that initiate haemostasis when a blood vessel is damaged. They form a temporary plug and support activation of the coagulation cascade, which stabilises the clot with fibrin. This system must remain finely balanced: insufficient clotting causes bleeding, while excessive clotting increases the risk of thrombosis, stroke, or pulmonary embolism.
All blood cells are produced in the bone marrow through haematopoiesis, guided by hormonal and immune signals such as erythropoietin from the kidneys. Because blood cells are continuously replaced, disruptions from nutritional deficiencies, medications, toxins, infection, or malignancy can rapidly alter blood composition. The spleen supports this system by filtering aged or abnormal cells and contributing to immune defence, helping maintain the quality and effectiveness of circulating blood.
Beyond the Basics
Haematology as a Multi-System Regulator
Haematology is the coordinated function of several organ systems rather than an isolated blood-cell factory. Red blood cell production depends on renal oxygen sensing, gastrointestinal absorption of nutrients, and bone marrow responsiveness. When oxygen delivery falls, the kidneys increase erythropoietin secretion, stimulating the bone marrow to increase erythropoiesis. In chronic kidney disease, this signal is reduced, leading to anaemia even when iron and vitamin stores are adequate.
Gastrointestinal health is equally critical. Iron, vitamin B12, and folate must be absorbed and transported to the bone marrow for haemoglobin synthesis and DNA replication during red cell maturation. Disruption at any point, renal, gastrointestinal, or marrow, reduces oxygen-carrying capacity and produces systemic hypoxia, fatigue, and reduced tissue function.
Haematology and Immune Integration
White blood cells form the mobile arm of the immune system, continuously moving between the blood, lymphatic tissues, and sites of injury or infection. Through cytokines and surface receptors, leukocytes coordinate inflammation, pathogen clearance, and adaptive immune memory.
When this regulatory system becomes dysbalanced, haematology becomes a driver of disease. In sepsis, excessive immune activation damages blood vessels, causes capillary leak, and disrupts coagulation, leading to organ failure. In autoimmune disease, inappropriate activation of white blood cells leads to tissue destruction. Modern immunotherapies such as monoclonal antibodies and CAR-T cell therapy demonstrate how manipulating haematological pathways can radically alter immune-mediated disease.
Coagulation as a Dynamic Balance System
Haemostasis is maintained by a tightly regulated interaction between platelets, clotting factors, and the vascular endothelium. This system must be sufficiently responsive to stop bleeding yet restrained enough to avoid thrombosis. Liver function, vitamin K availability, inflammatory mediators, and blood flow all influence this balance. Because clotting factors are proteins produced in the liver and activated through enzymatic cascades, systemic illness, malnutrition, liver disease, or medications can shift the system toward bleeding or clotting. Even dehydration or immobility increases blood viscosity and alters coagulation dynamics, raising thrombotic risk without any primary blood disorder.
Blood Transfusion and Systemic Impact
Blood transfusion illustrates how deeply haematology is integrated into whole-body physiology. Transfused red cells alter oxygen delivery, plasma volume, and blood viscosity, while plasma products affect coagulation and immune interactions. For this reason, transfusion is a powerful but potentially disruptive therapy.
Safe transfusion depends on careful compatibility testing, controlled storage, and close patient monitoring. Although transfusion can be life-saving, it can also trigger immune reactions, haemolysis, volume overload, or inflammatory responses, highlighting why haematological interventions must always be considered in the context of the entire cardiovascular and immune systems.
Clinical Connections
Changes in blood composition are often the earliest and most sensitive indicators of physiological stress, disease progression, or treatment-related complications. Blood results frequently shift before vital signs deteriorate, making them an early warning system in acute care, chronic disease, and oncology settings.
Red blood cell abnormalities directly impair oxygen delivery. Falling haemoglobin or abnormal red cell indices help explain symptoms such as fatigue, dyspnoea, dizziness, delayed wound healing, and reduced exercise tolerance. Recognising patterns allows clinicians to distinguish between iron deficiency, chronic disease, renal anaemia, or acute blood loss and to guide timely interventions such as iron therapy, vitamin replacement, or escalation of care.
White blood cell changes provide critical insight into immune function and inflammatory status. A rising neutrophil count may signal bacterial infection or physiological stress, while lymphopenia can indicate immune suppression or severe illness. Abnormal or immature cells may suggest bone marrow disease. Early interpretation supports rapid identification of sepsis, treatment-related immunosuppression, or haematological malignancy before overt clinical decline.
Platelet and coagulation abnormalities influence both bleeding and clotting risk, which has immediate implications for procedures, anticoagulant use, and patient safety. Declining platelets increase the risk of haemorrhage, while elevated clotting activity increases the risk of thrombosis, stroke, or pulmonary embolism.
Key haematological patterns that guide clinical decisions include:
falling haemoglobin indicating blood loss or marrow failure
rising or falling white cell counts reflecting infection, inflammation, or immunosuppression
abnormal platelets or coagulation studies signalling bleeding or clotting risk
Systemic illness and medical treatments frequently manifest first in the blood. Liver disease alters clotting factor production, renal failure reduces erythropoietin and causes anaemia, chemotherapy suppresses bone marrow activity, and severe infection disrupts all blood cell lines. Monitoring these changes allows clinicians to anticipate complications rather than simply react to them.
Most importantly, trends matter more than isolated values. Serial full blood counts, coagulation profiles, and iron studies show whether a patient is stabilising, responding to therapy, or deteriorating. This makes haematology a central tool in risk stratification, escalation planning, and safe ongoing care across almost every clinical setting.
Concept Check
Explain how red blood cells are produced in the bone marrow and how erythropoietin regulates this process.
How do white blood cells contribute to immunity, and why might abnormal counts indicate infection or malignancy?
Describe the steps involved in haemostasis and explain what can go wrong in bleeding or clotting disorders.
Why are patients with chronic kidney disease at high risk of anaemia, and how is this linked to haematological physiology?
A patient presents with fatigue, pallor, shortness of breath, and spoon-shaped nails. Which haematological condition should you suspect, and what tests would be relevant?