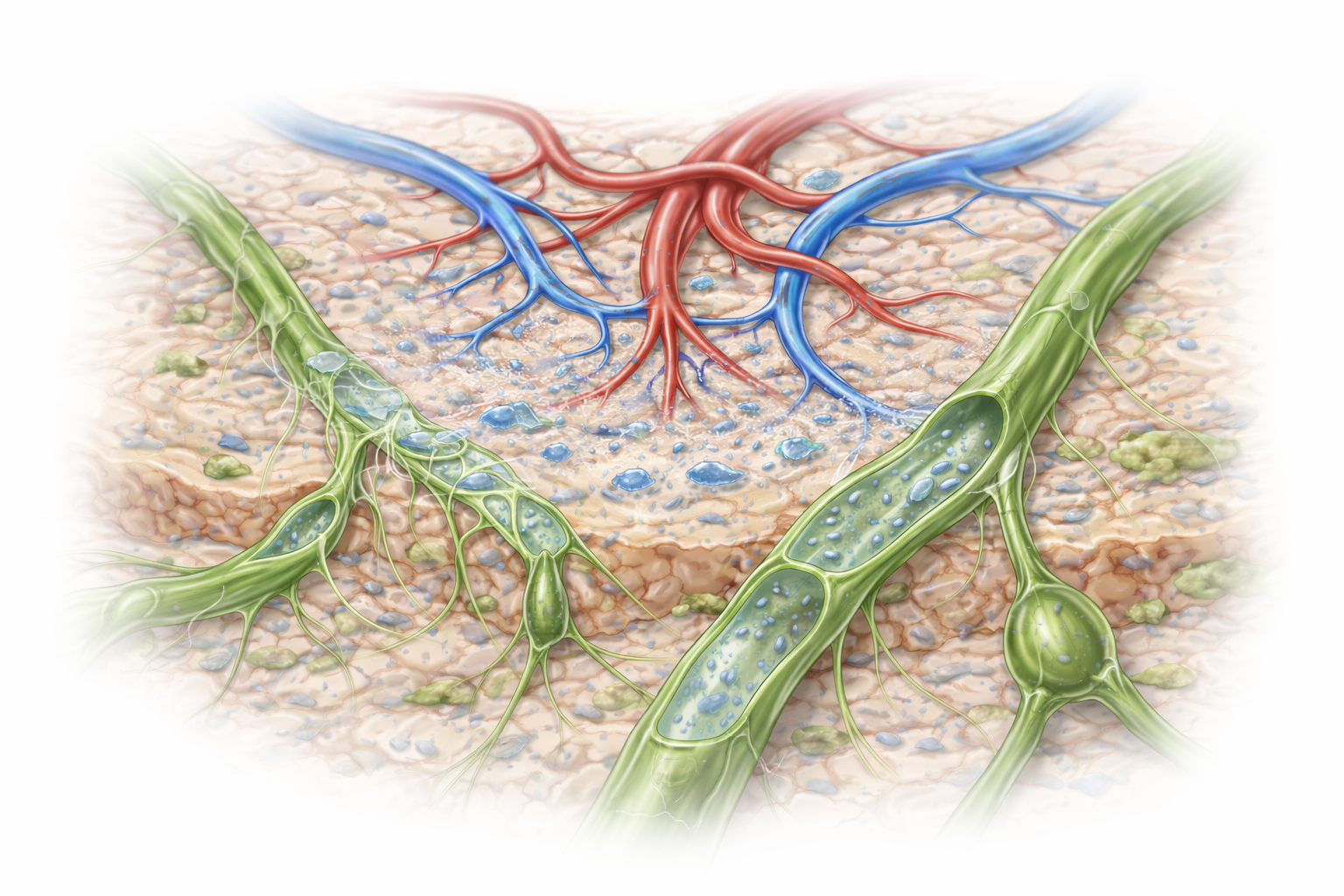
LYMPH FORMATION & RETURN TO CIRCULATION
The lymphatic system plays a crucial role in maintaining fluid balance by returning excess interstitial fluid, plasma proteins and waste products back into the bloodstream. This process prevents tissue swelling, supports nutrient exchange and enables continuous immune surveillance. Lymph formation and return to circulation depend on specialised lymphatic capillaries, pressure gradients and coordinated vessel function. Without this system, even normal cardiovascular filtration would rapidly lead to oedema and impaired tissue function.
What You Need to Know
Lymph formation is a normal consequence of capillary fluid exchange. As blood flows through capillaries, hydrostatic pressure drives fluid out into the interstitial space to deliver oxygen, nutrients, and signalling molecules to tissues. While most of this fluid is reabsorbed at the venous end of the capillary, a portion remains in the interstitial space. This excess fluid enters nearby lymphatic capillaries and is then referred to as lymph.
Several key processes define lymph formation and movement:
Entry of excess interstitial fluid, proteins, and cellular debris into lymphatic capillaries
One-way transport through lymphatic vessels aided by valves, skeletal muscle contraction, and pressure changes during breathing
Filtration through lymph nodes, where pathogens and debris are removed and immune cells interact
Return of lymph to the bloodstream via the thoracic duct or right lymphatic duct
Once inside the lymphatic system, lymph moves through progressively larger vessels and passes through lymph nodes positioned along its path. These nodes act as checkpoints where antigens are sampled and immune responses can be initiated. This constant circulation allows immune cells to traffic between tissues and lymphoid organs, supporting immune surveillance.
Return of lymph to the venous circulation is essential for maintaining fluid balance. By reclaiming excess interstitial fluid, the lymphatic system prevents tissue oedema, returns leaked plasma proteins to the bloodstream, and transports absorbed dietary lipids from the gastrointestinal tract. Lymph formation and return therefore play a critical role in fluid homeostasis, immune defence, and normal tissue function.
Image: Fluid filters out of blood capillaries into the surrounding tissue, forming interstitial fluid. Most is reabsorbed at the venous end, but excess fluid enters nearby lymphatic capillaries through overlapping endothelial flaps, becoming lymph and returning to the circulation.
Beyond the Basics
How Interstitial Fluid Becomes Lymph
Lymph formation begins at the level of blood capillaries, where fluid exchange is driven by pressure gradients. Hydrostatic pressure within capillaries pushes plasma fluid out into surrounding tissues to support nutrient delivery and waste removal. While most of this fluid is reabsorbed at the venous end through osmotic forces, a small but significant proportion remains within the interstitial space.
Lymphatic capillaries are designed to collect this excess fluid efficiently. Their walls are composed of overlapping endothelial cells that function as one-way microvalves. When interstitial pressure rises, these valves open inward, allowing fluid, plasma proteins, immune cells, and even larger particles such as bacteria to enter. Once inside, the valves close, preventing backflow. This structure allows the lymphatic system to clear material that cannot be reabsorbed directly into blood capillaries, maintaining tissue fluid balance and preventing oedema.
Transport Through Lymphatic Vessels
After entering lymphatic capillaries, lymph is directed into progressively larger collecting vessels. These vessels resemble veins in structure and contain internal valves that enforce one-directional flow toward the central circulation. Unlike the cardiovascular system, the lymphatic system does not have a central pump.
Instead, lymph movement relies on several coordinated forces:
Skeletal muscle contraction compresses lymphatic vessels during movement
Respiratory pressure changes draw lymph toward the thoracic cavity during inspiration
Rhythmic contraction of smooth muscle within lymphatic vessel walls propels lymph forward
Arterial pulsation assists lymph movement in vessels running alongside arteries
Together, these mechanisms generate a slow but continuous flow that adapts to changes in activity, posture, and breathing.
Movement Through Lymph Nodes
As lymph travels through the lymphatic network, it passes through lymph nodes positioned along major vessels. Within these nodes, lymph flows through a series of sinuses lined with macrophages and dendritic cells. These immune cells trap pathogens, cellular debris, and foreign particles while lymphocytes survey antigens carried in the lymph.
This filtration process serves two purposes. Harmful material is removed before lymph returns to circulation, and antigens are presented to immune cells, allowing initiation of adaptive immune responses when needed. Lymph nodes therefore act as both mechanical filters and immunological checkpoints.
Return of Lymph to the Venous Circulation
Filtered lymph ultimately drains into one of two major lymphatic ducts that return fluid to the bloodstream. The thoracic duct is the larger of the two and drains lymph from both lower limbs, the abdomen, the left side of the thorax, the left arm, and the left side of the head and neck. It empties into the left subclavian vein.
The right lymphatic duct drains lymph from the right arm, right side of the thorax, and right side of the head and neck, returning it to the right subclavian vein. Together, these ducts return several litres of lymph to the venous circulation each day, preserving plasma volume and preventing fluid loss from tissues.
Composition and Variability of Lymph
Lymph composition varies depending on its tissue of origin. Peripheral lymph is relatively clear and contains water, plasma proteins, electrolytes, and immune cells. In contrast, lymph draining from the gastrointestinal tract contains a high concentration of absorbed dietary fats packaged into chylomicrons. This lipid-rich lymph, known as chyle, has a milky appearance and is essential for fat transport.
Through continuous lymph return, the lymphatic system maintains plasma protein levels, supports nutrient distribution, and stabilises circulatory volume. Disruption at any stage of this process can lead to tissue swelling, impaired immunity, or altered nutrient absorption.
Clinical Connections
Disruption of lymph formation or lymphatic flow leads to accumulation of interstitial fluid and development of lymphoedema. This condition arises when lymphatic vessels are unable to return fluid to the circulation at a rate that matches capillary filtration. Unlike simple oedema, lymphoedema is characterised by protein-rich fluid accumulation, progressive tissue swelling, and increased risk of skin infection due to impaired immune surveillance.
Common clinical situations associated with impaired lymphatic function include:
Surgical removal or damage to lymph nodes, particularly following cancer treatment
Radiation therapy causing fibrosis and obstruction of lymphatic vessels
Tumour compression of lymphatic channels
Recurrent infection or inflammation that damages lymphatic structure
Systemic conditions can also overwhelm lymphatic capacity. Congestive heart failure increases capillary hydrostatic pressure, driving excess fluid into the interstitial space. Severe hypoalbuminaemia reduces plasma oncotic pressure, limiting reabsorption of fluid back into capillaries. In both situations, lymphatic drainage may be intact but insufficient to manage the increased fluid load, resulting in oedema.
Differentiating lymphoedema from venous oedema guides appropriate management and referral. Knowledge of lymphatic flow patterns informs safe use of compression therapy and manual lymphatic drainage, which rely on directing fluid toward functioning lymphatic pathways. Accurate recognition of lymphatic dysfunction supports effective symptom management, infection prevention, and long-term tissue health.
Concept Check
What causes interstitial fluid to enter lymphatic capillaries?
Why does lymph require valves to move effectively through vessels?
How do skeletal muscle contractions and breathing influence lymph flow?
Which regions of the body drain into the thoracic duct versus the right lymphatic duct?
What is chyle, and how does it differ from typical lymph?