OVARIAN STRUCTURE & FOLLICULOGENESIS
The ovaries are specialised reproductive organs that house oocytes and support their maturation through the process of folliculogenesis. Understanding ovarian structure and follicular development is essential for interpreting normal menstrual cycles, fertility, hormonal regulation and conditions such as anovulation, polycystic ovary syndrome and ovarian insufficiency.
THE MENSTRUAL CYCLE: Endocrine Regulation, Ovarian Dynamics and Cyclical Endometrial Change
The menstrual cycle is a cyclic, hormonally regulated process involving coordinated changes in the hypothalamus, pituitary gland, ovaries and endometrium that prepare the body for potential fertilisation and pregnancy. Understanding this process is essential for interpreting normal reproductive physiology, fertility, menstrual disorders and endocrine dysfunction across the female lifespan.
OOGENESIS: Development and Maturation of the Female Gamete Across the Lifespan
Oogenesis is the process by which female gametes develop and mature, beginning before birth and progressing through prolonged periods of arrest until selected oocytes resume development during the reproductive years. Understanding oogenesis is essential for interpreting fertility, age-related reproductive decline, chromosomal abnormalities and disorders of female reproductive development.
THE UTERUS: Structure & Function
The uterus is a hollow, muscular organ whose layered structure is specialised to support implantation, menstrual cycling, pregnancy and childbirth. Understanding the anatomy and function of the uterine wall is essential for interpreting fertility, menstrual physiology, early pregnancy, contraception and common gynaecological conditions.
THE CERVIX: Structure & Function
The cervix is the lower portion of the uterus that forms the passage between the uterine cavity and the vagina, with a structure specialised for barrier protection, sperm transport and mechanical support. Understanding cervical anatomy and function is essential for interpreting fertility, infection risk, cervical screening, pregnancy maintenance and the physiological changes that allow labour and childbirth.
THE VAGINA: Structure & Function
The vagina is a muscular, elastic canal that connects the cervix to the external genitalia and functions as a conduit for menstruation, sexual intercourse and childbirth. Understanding its structure and microenvironment is essential for interpreting reproductive health, infection risk, sexual function, hormonal influences and obstetric care.
FEMALE EXTERNAL GENITALIA (VULVA): Structure & Function
The vulva comprises the external genital structures of the female reproductive system and functions to protect the internal reproductive tract while supporting urination, sexual function, arousal and the entry of sperm. Understanding vulvar anatomy is essential for interpreting sexual health, infection risk, hormonal changes, trauma, urogynaecological conditions and normal variation across the lifespan.
PREGNANCY PHYSIOLOGY (MATERNAL ADAPTATIONS)
Pregnancy physiology refers to the adaptations that support fetal growth, maintain maternal health and prepare the body for labour and birth. Understanding these normal physiological changes is essential for interpreting clinical findings in pregnancy, distinguishing expected adaptations from pathology and providing safe, informed antenatal care.
THE PLACENTA: Structure & Function
Placental structure and function describe how this temporary organ supports fetal growth by facilitating nutrient and gas exchange, waste removal and endocrine signalling between maternal and fetal circulations. Understanding the placenta is essential for interpreting normal pregnancy physiology, fetal development and the pathophysiology of pregnancy complications.
THE BREAST: Physiology & Lactation
Lactation and breast physiology describe how the mammary glands produce and deliver breast milk through coordinated hormonal, neural and structural mechanisms. Understanding this process is essential for supporting infant nutrition, maternal health and early mother–infant bonding, and for recognising common lactation difficulties.
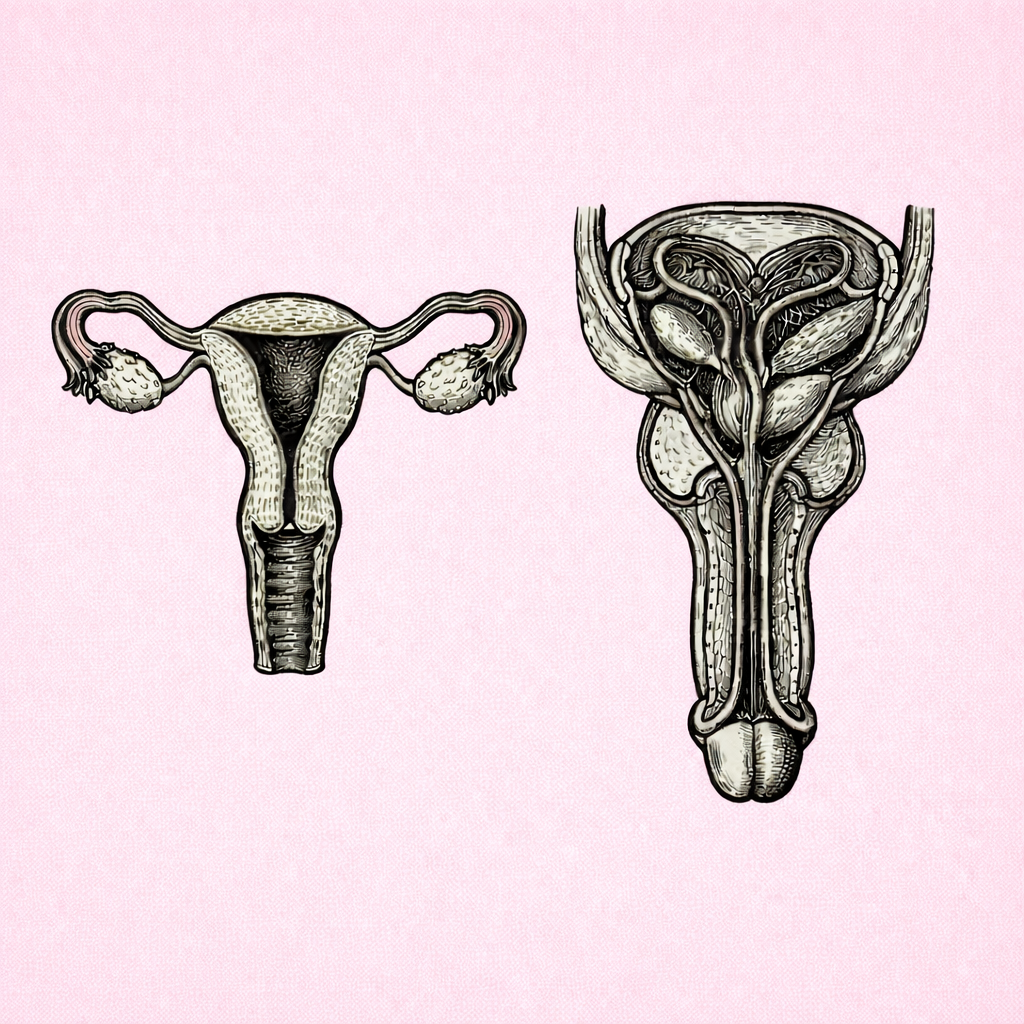
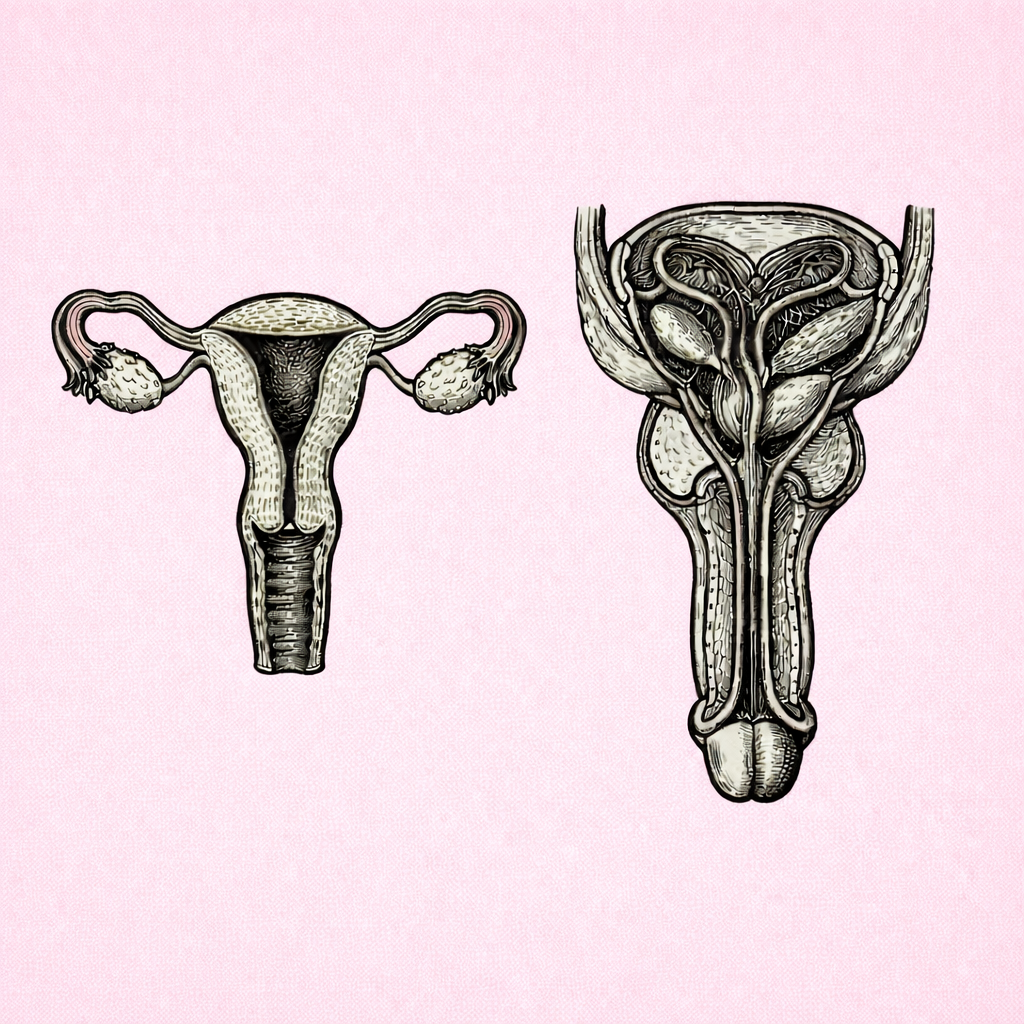
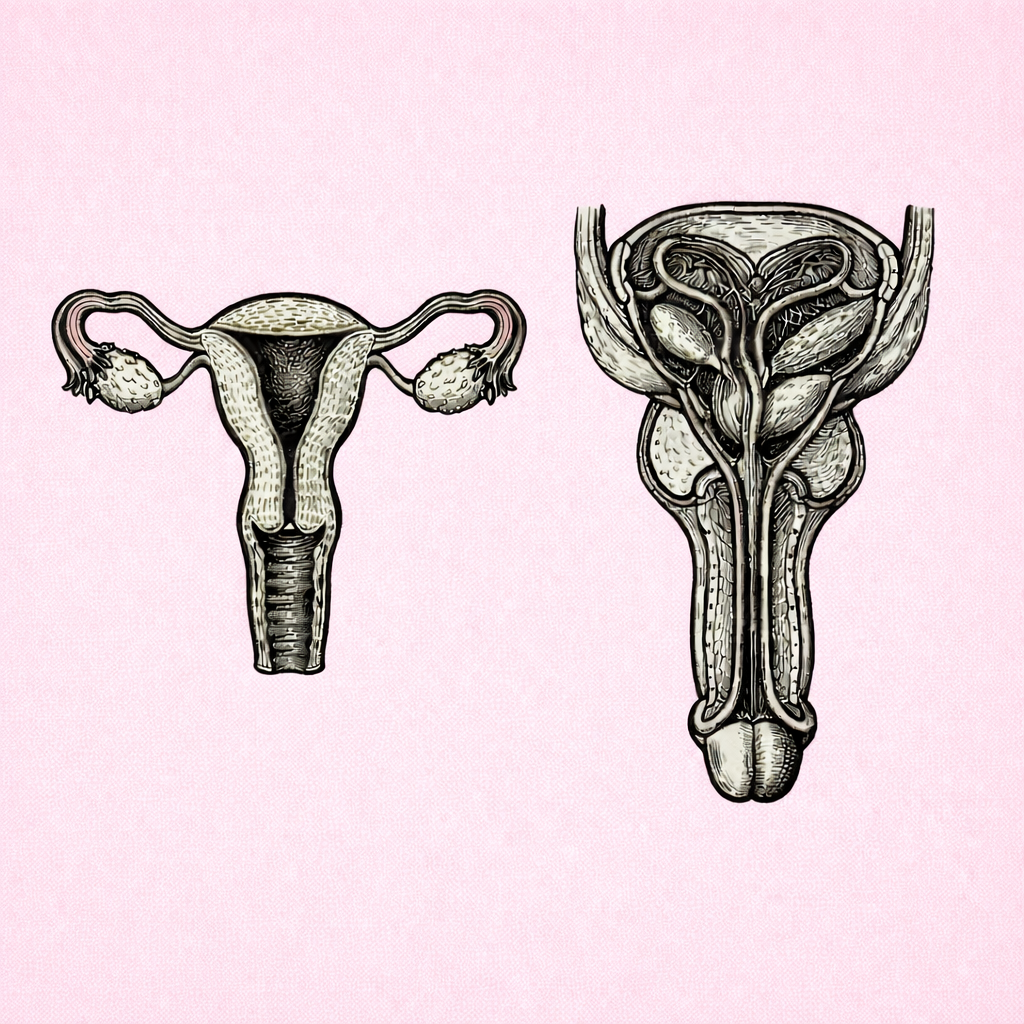
TESTICULAR STRUCTURE & SPERMATOGENESIS
Testicular structure and spermatogenesis describe how the testes are organised to produce sperm and testosterone through tightly regulated hormonal, thermal and cellular mechanisms. Understanding this process is essential for interpreting male fertility, reproductive development, endocrine disorders and the effects of disease or environmental factors on sperm production.
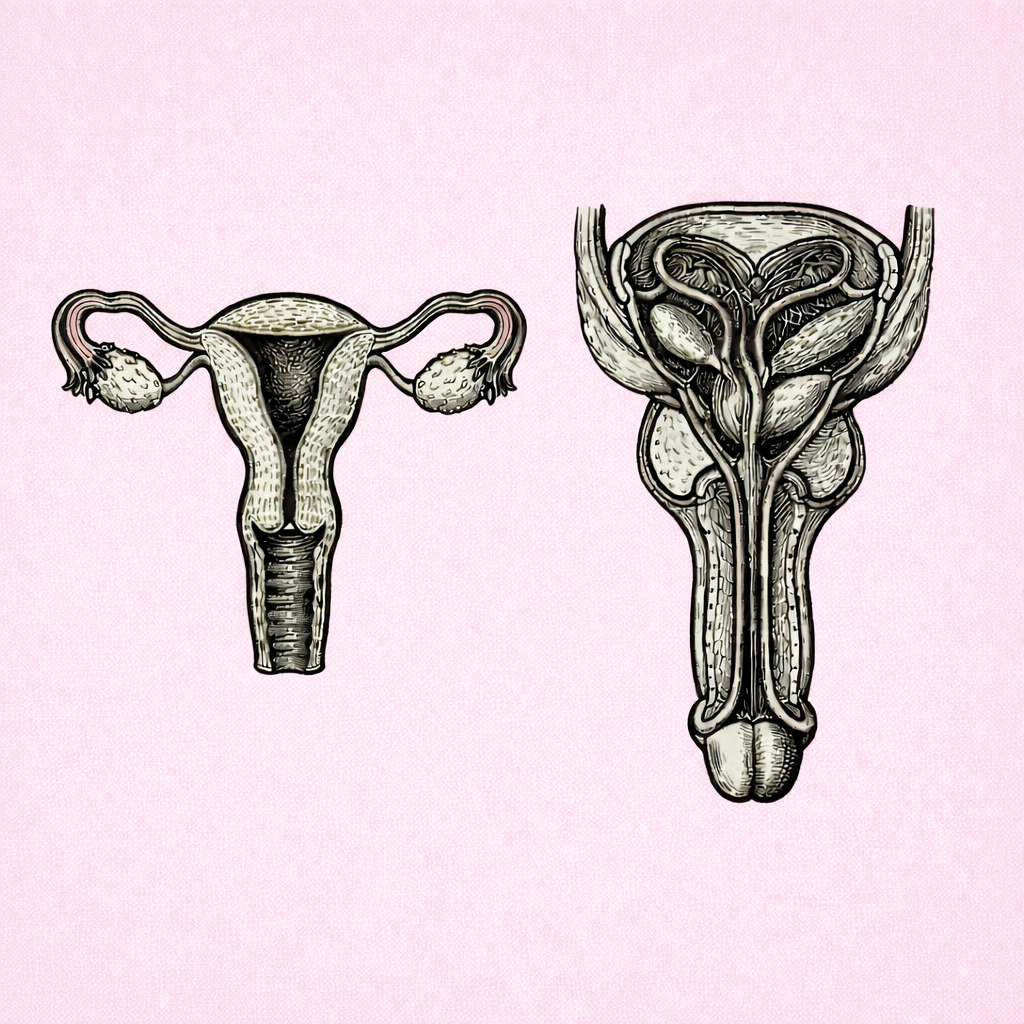
MALE REPRODUCTIVE DUCT SYSTEM
The male reproductive duct system is a series of interconnected passages that transport sperm from the testes to the exterior of the body, while supporting their maturation, storage and delivery. Understanding this pathway explains how sperm become capable of fertilisation and underpins clinical concepts such as male fertility, reproductive health and surgical contraception.
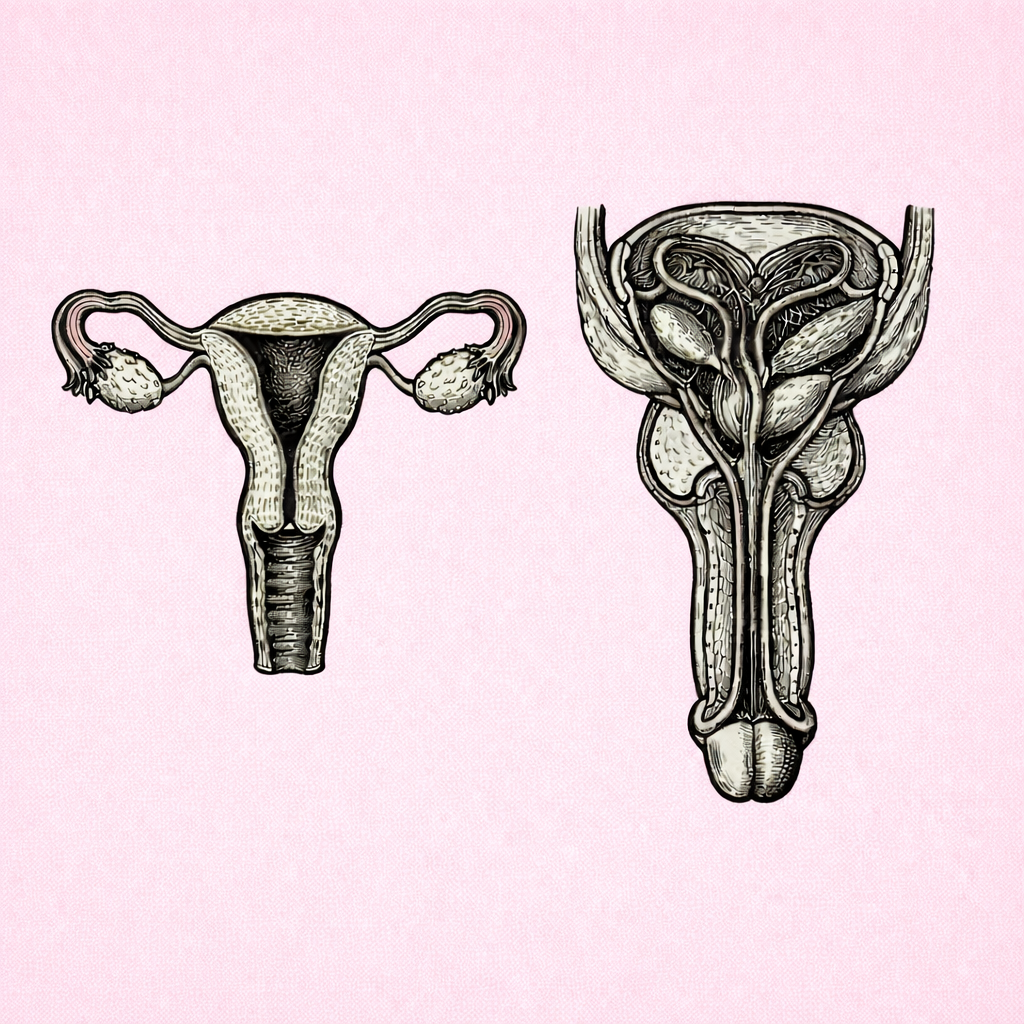
MALE REPRODUCTIVE SYSTEM: Accessory Glands
The accessory glands of the male reproductive system produce the fluid components of semen that nourish sperm, support motility and protect them within the female reproductive tract. Understanding the roles of the seminal vesicles, prostate gland and bulbourethral glands explains how functional semen is formed and informs fertility, prostate health and reproductive disorders.
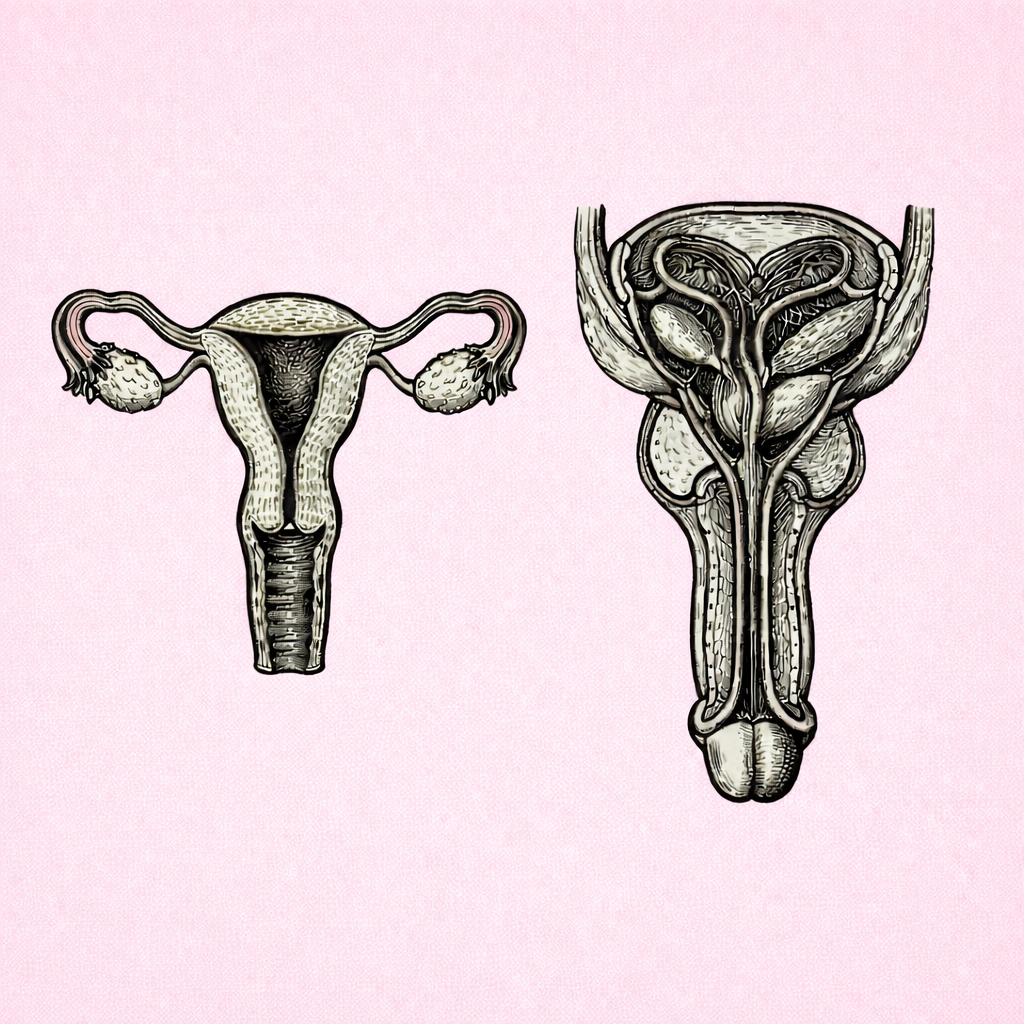
HORMONAL REGULATION OF MALE REPRODUCTION
Male reproductive function is regulated by the hypothalamic–pituitary–gonadal (HPG) axis, which controls sperm production, testosterone synthesis and sexual development through coordinated hormonal signalling. Understanding this regulation is essential for interpreting disorders of puberty, fertility, sexual function and endocrine pathology.
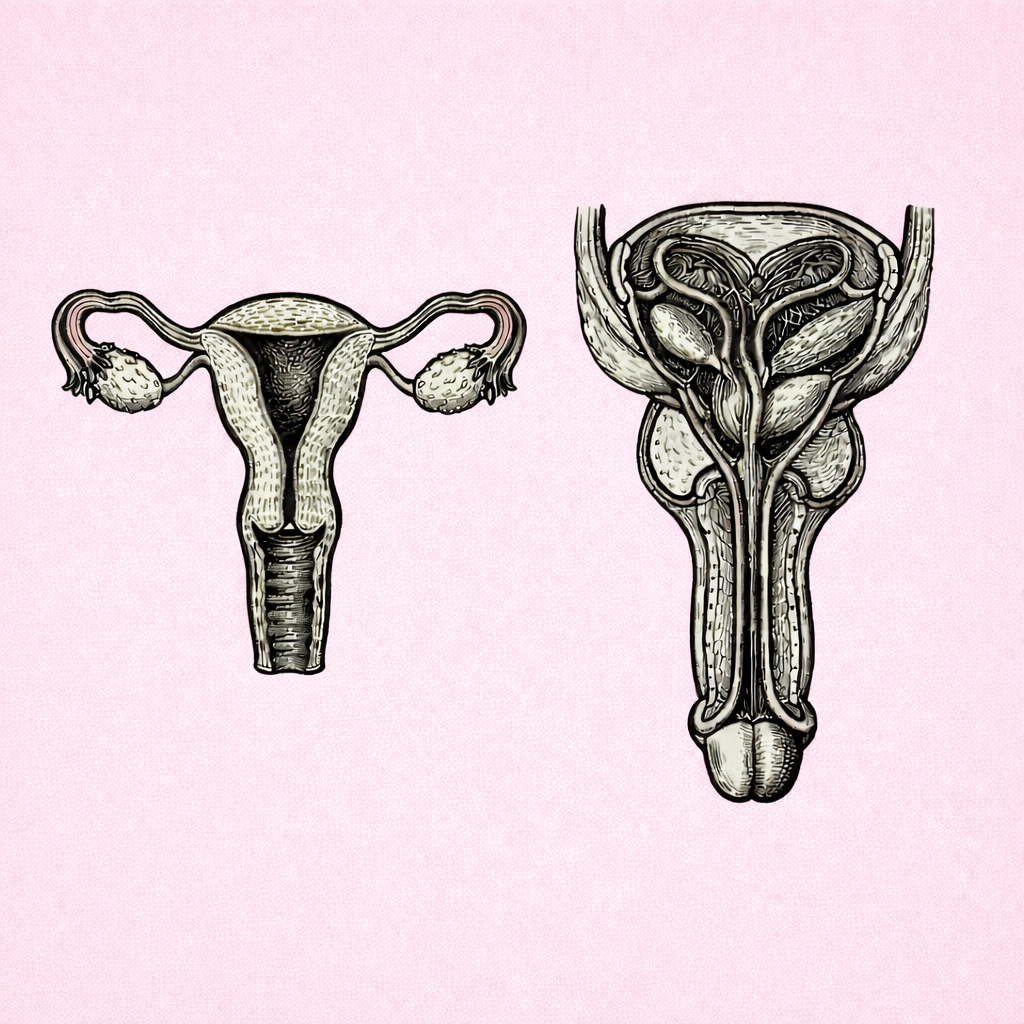
PENILE ANATOMY & PHYSIOLOGY
The penis is a specialised organ that integrates vascular, neural and connective tissue structures to enable urination, sexual function, erection and ejaculation. Understanding its anatomy and physiology is essential for interpreting erectile function, sexual health, male fertility and disorders such as erectile dysfunction.
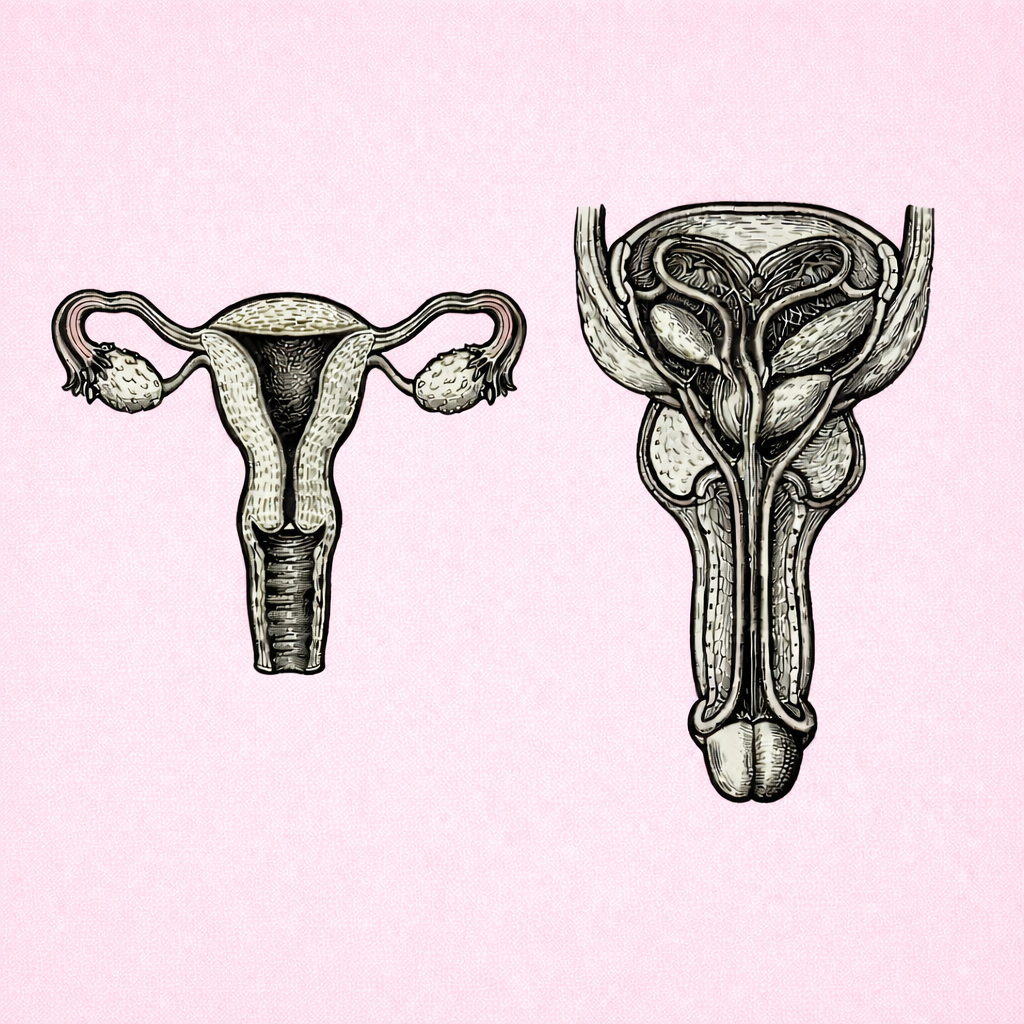
ESTROGEN: Structure, Functions and Physiological Roles Across the Lifespan
Estrogen is a key steroid hormone that regulates ovarian function, the menstrual cycle, fertility and the development of secondary sexual characteristics, while also influencing bone, cardiovascular, metabolic and neurological health. Understanding estrogen physiology is essential for interpreting menstrual regulation, contraception, fertility, pregnancy-related changes and the transitions of menopause across the lifespan.
PROGESTERONE: Structure, Functions and Central Role in Menstrual Physiology and Early Pregnancy
Progesterone is a steroid hormone that regulates the second half of the menstrual cycle and prepares the uterus for implantation and early pregnancy. Understanding progesterone is essential for interpreting ovulation, menstrual regulation, fertility, early pregnancy maintenance and disorders of reproductive and hormonal balance.
LUTEINISING HORMONE (LH): Key Regulator of Ovulation
Luteinising hormone (LH) is a pituitary hormone that regulates ovulation in females and testosterone production in males. Understanding LH is essential for interpreting fertility, ovulatory function, menstrual cycle regulation and disorders of the hypothalamic–pituitary–gonadal axis.
ANTI-MÜLLERIAN HORMONE (AMH)
Anti-Müllerian hormone (AMH) is a reproductive hormone produced by ovarian granulosa cells that reflects follicle activity and ovarian reserve. Understanding AMH is important for interpreting fertility potential, ovarian ageing, and conditions such as PCOS and premature ovarian insufficiency, as well as its role in male fetal sexual differentiation.
PROLACTIN: Hormone of Lactation, Reproductive Regulation and Neuroendocrine Function
Prolactin is a pituitary hormone best known for its role in initiating and maintaining lactation, with additional effects on reproduction, metabolism, immune function and behaviour. Understanding prolactin is important for interpreting fertility disturbances, menstrual irregularities, sexual dysfunction and disorders of pituitary regulation.