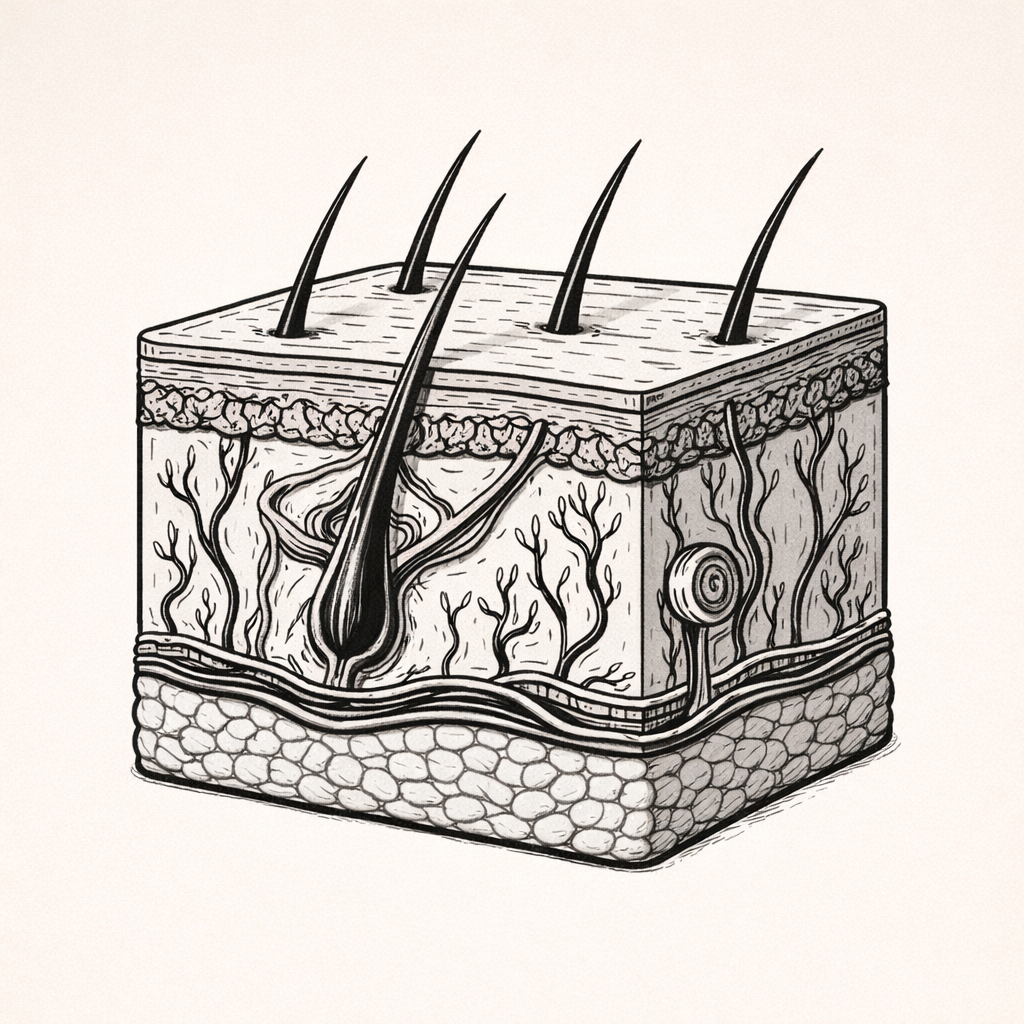
Age-Related Skin Changes
Age-related skin changes involve progressive structural and functional alterations across all layers of the integumentary system. Understanding these changes is essential for recognising increased risk of skin injury, impaired wound healing, infection, and complications associated with ageing in clinical practice.
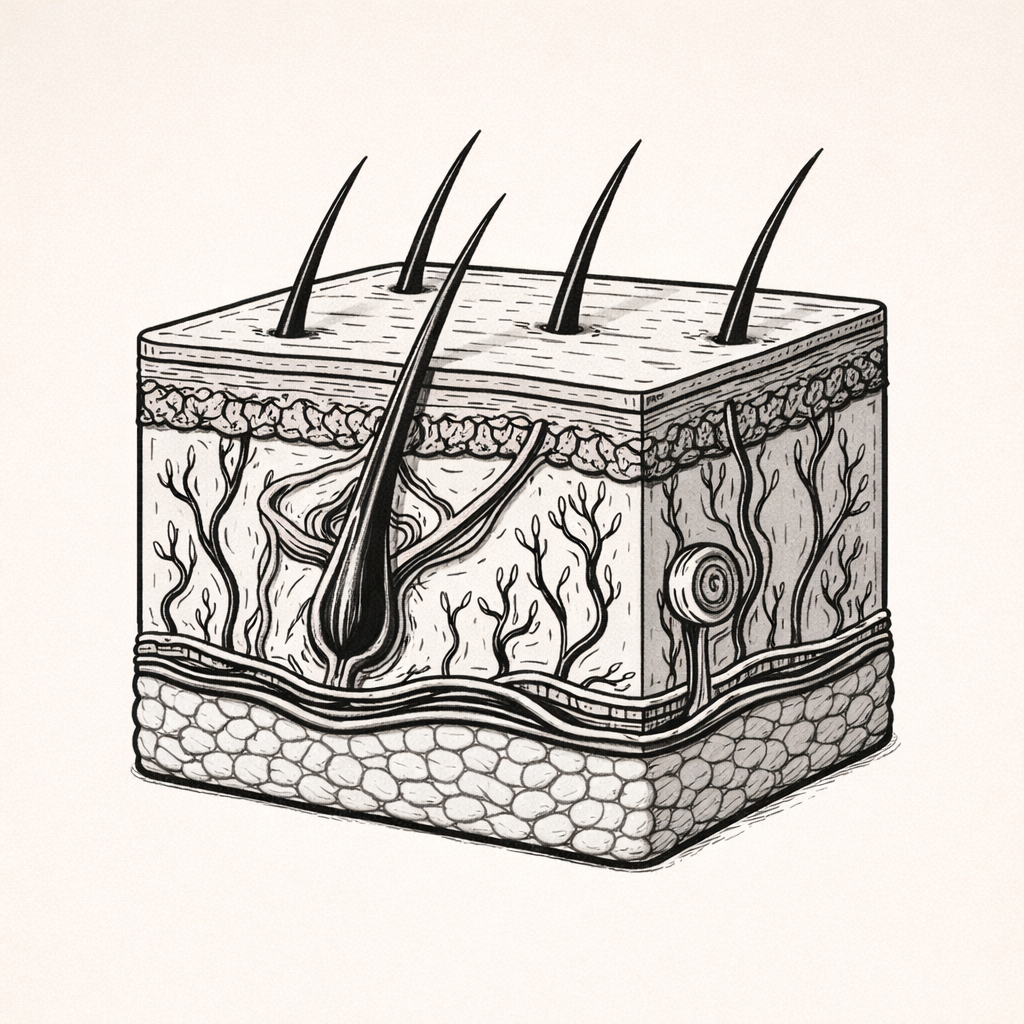
Mechanical Properties of Skin: Elasticity, Tensile Strength, Viscoelasticity and Structural Adaptation
The mechanical properties of skin describe how it stretches, resists force, and recovers shape through the coordinated structure of collagen, elastin, and dermal matrix components. Understanding these properties is essential for explaining pressure injury development, scarring, skin ageing, and the skin’s response to mechanical stress in clinical care.
Sweat & Sebaceous Glands
Sweat and sebaceous glands are specialised skin structures that support thermoregulation, barrier protection, and microbial defence. Understanding how these glands function is essential for explaining temperature control, hydration, electrolyte balance, and disorders affecting skin integrity and homeostasis.
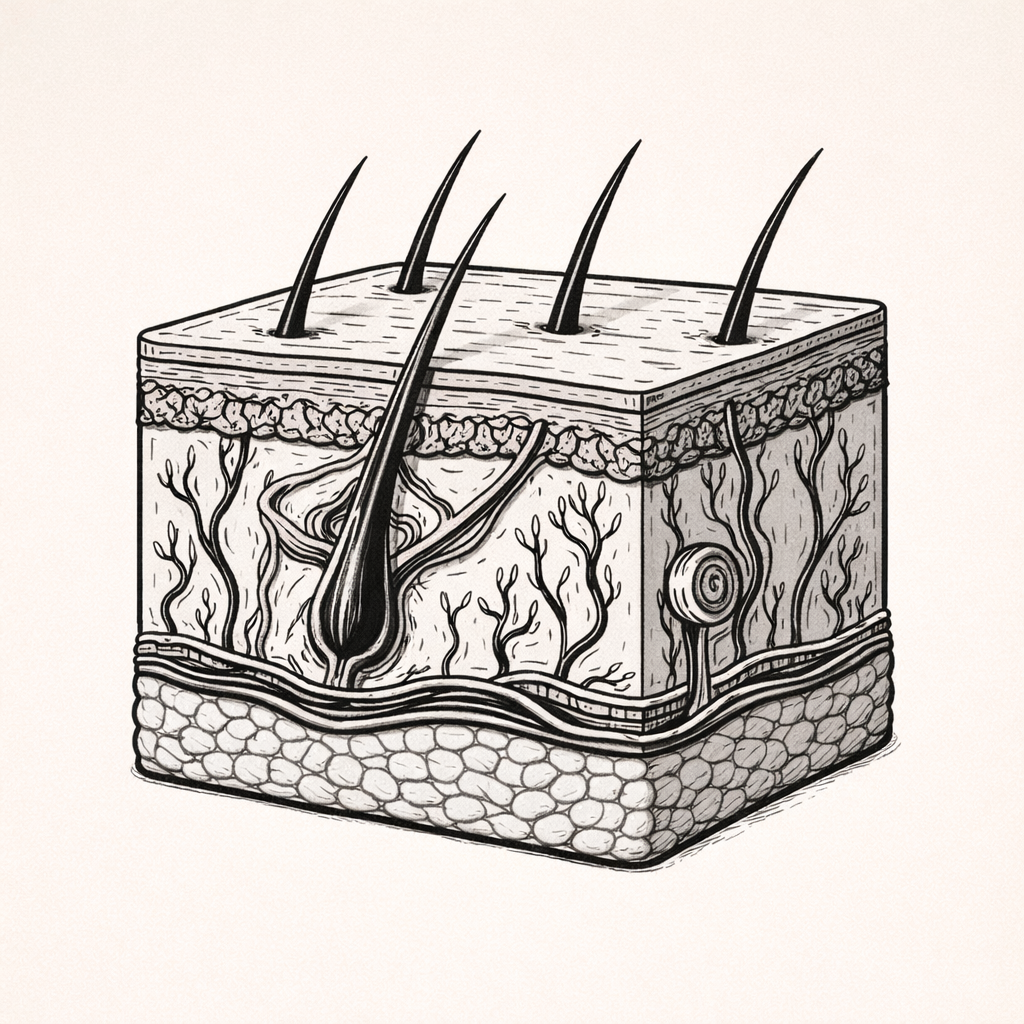
Acid Mantle & Barrier Function
The acid mantle and barrier function describe how the skin protects the body through an integrated chemical, physical, and immunological defence system. Understanding these mechanisms is essential for preventing infection, managing wound care, reducing water loss, and supporting skin integrity in clinical practice.
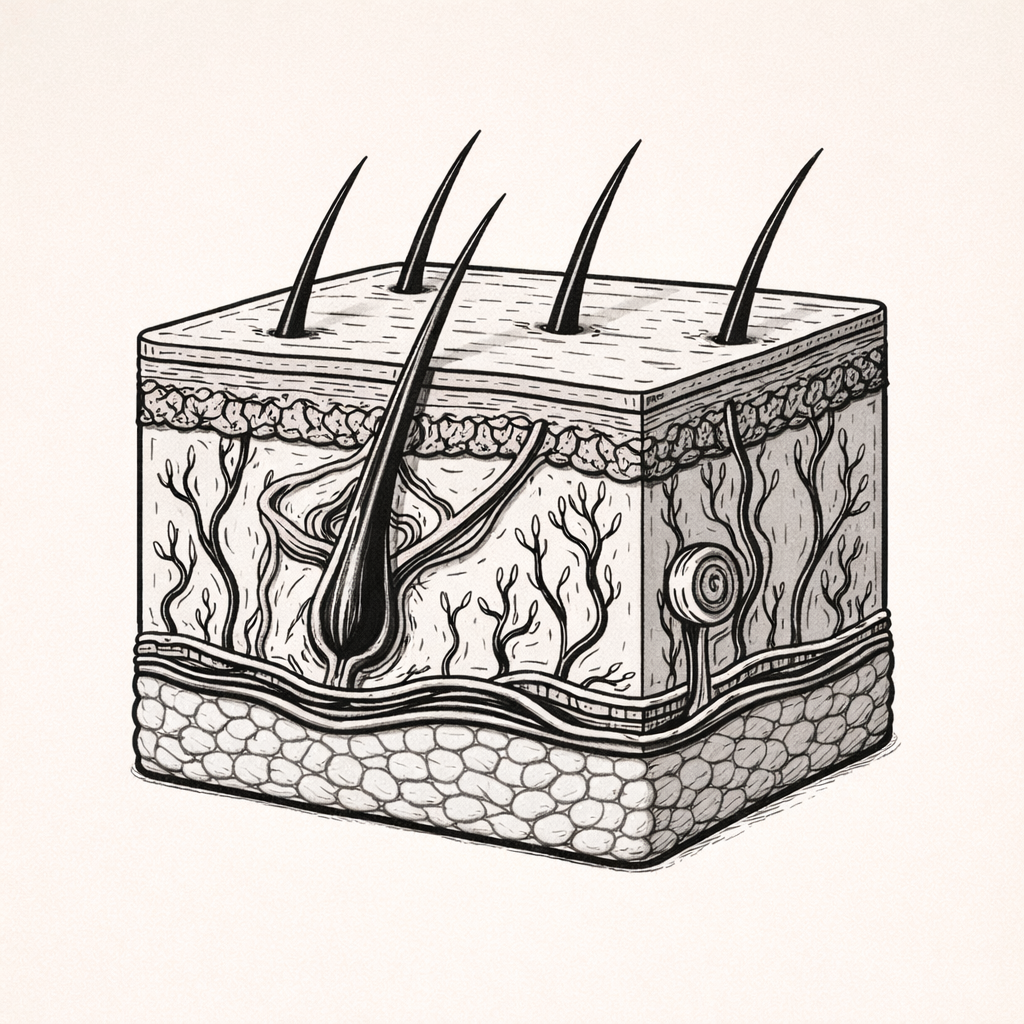
Keratinocyte Lifecycle
The keratinocyte lifecycle describes the regulated process by which epidermal cells proliferate, differentiate, and form the skin’s protective barrier. Understanding this cycle is essential for explaining normal skin renewal, wound healing, and the pathophysiology of dermatological disease.
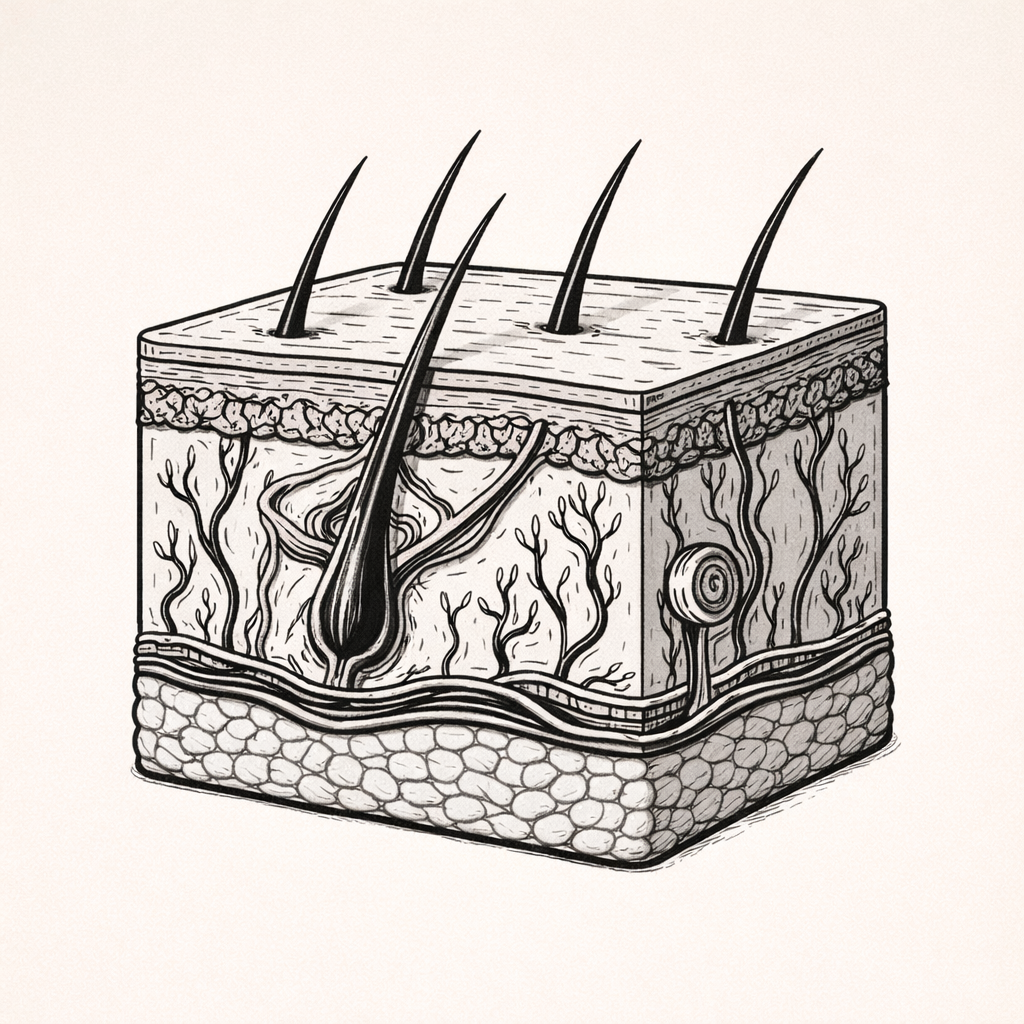
Vitamin D Synthesis
Vitamin D synthesis is a process in which the skin acts as an endocrine organ to initiate production of biologically active vitamin D. Understanding this pathway is essential for explaining calcium regulation, bone health, immune function, and the influence of sunlight and skin factors on vitamin D status.
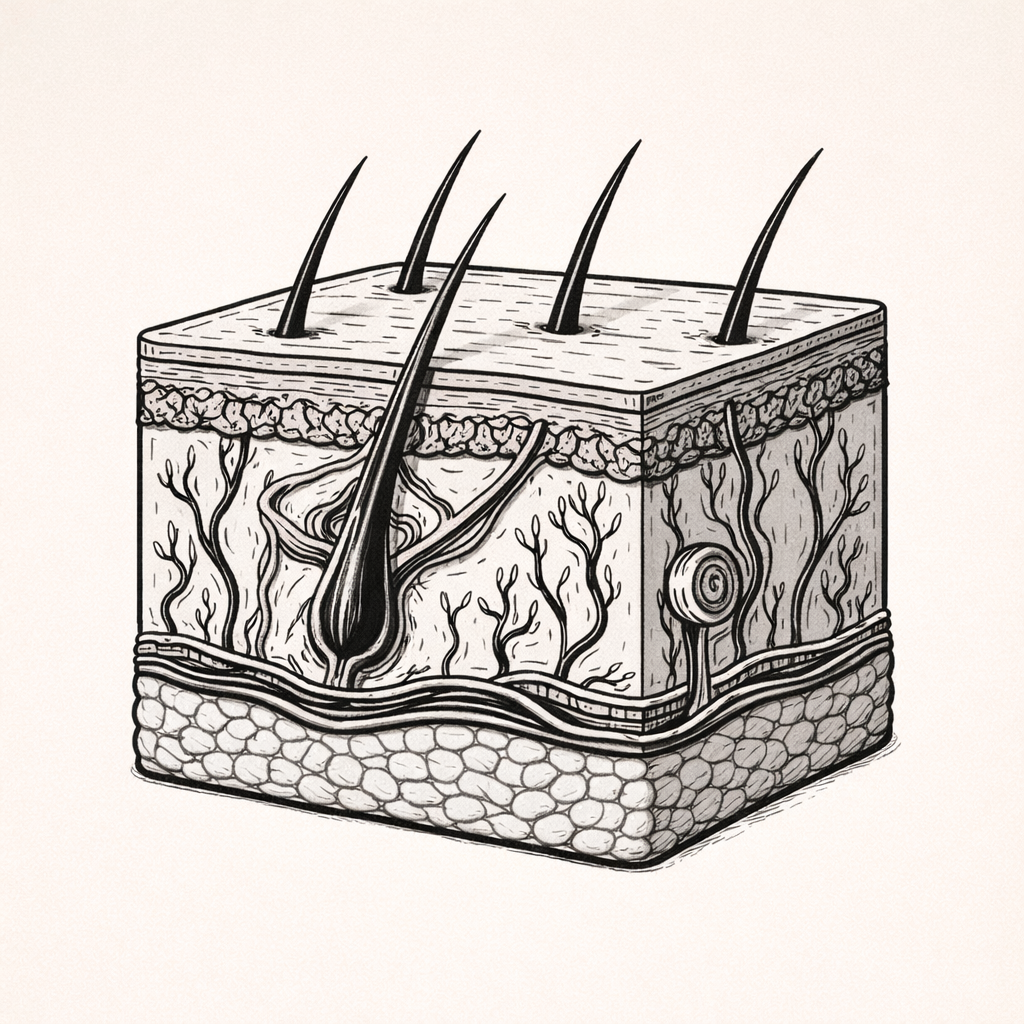
WOUND HEALING — Stage 2: Inflammation
The inflammatory stage of wound healing is a tightly regulated phase that recruits immune cells to control infection and prepare tissue for repair. Understanding this stage is essential for recognising why wounds either progress normally or become chronic when inflammation is insufficient, excessive, or prolonged.
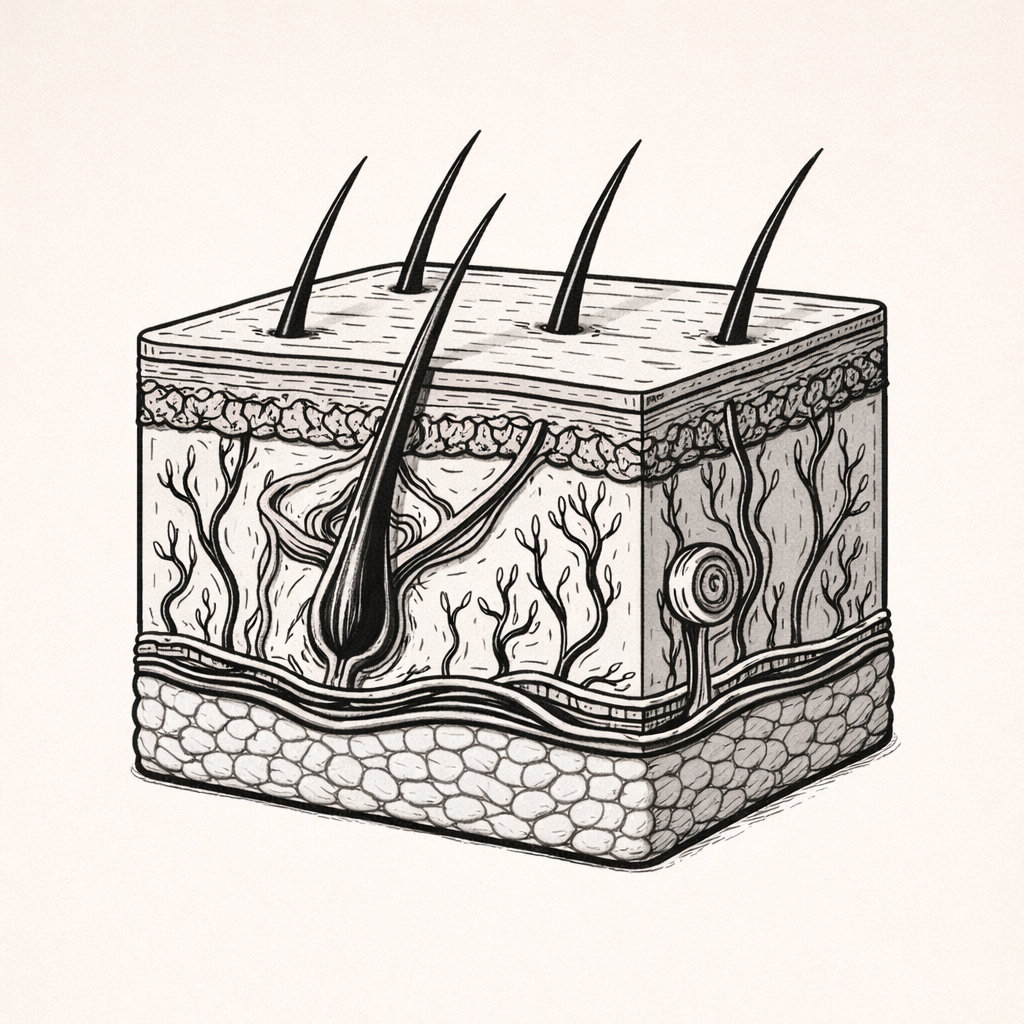
WOUND HEALING — Stage 3: Proliferation
The proliferative stage of wound healing is the phase in which new tissue is actively formed through granulation, angiogenesis, re-epithelialisation, and wound contraction. Understanding this stage is essential for recognising healthy healing progression and identifying factors that compromise tissue strength, barrier restoration, and long-term wound outcomes.
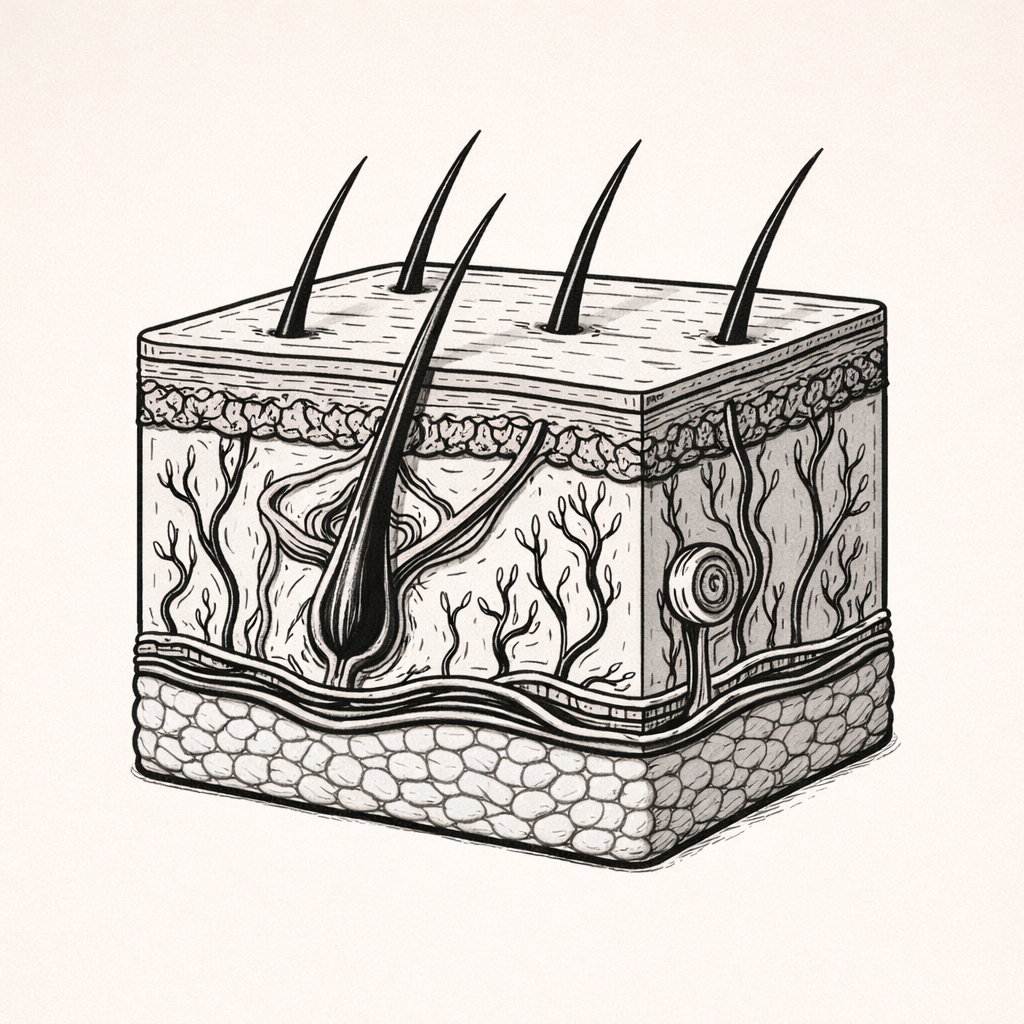
WOUND HEALING — Stage 4: Remodelling (Maturation)
The remodelling stage of wound healing is the final phase in which newly formed tissue is reorganised and strengthened into a mature scar. Understanding this stage is essential for explaining long-term wound strength, scar formation, and why healed skin never fully regains its original tensile integrity.
WOUND HEALING — Stage 1: Haemostasis
Haemostasis is the initial stage of wound healing in which bleeding is rapidly controlled through clot formation and vessel constriction. Understanding this stage is essential for explaining how wounds are stabilised, protected from contamination, and biologically primed for subsequent inflammation and tissue repair.
Specialised Epidermal Cells: Keratinocytes, Melanocytes, Langerhans Cells and Merkel Cells
Specialised epidermal cells include keratinocytes, melanocytes, Langerhans cells, and Merkel cells, each contributing distinct structural, immune, pigmentary, and sensory functions. Understanding these cell types is essential for interpreting normal skin physiology and recognising disorders of pigmentation, immune defence, sensation, and barrier integrity.
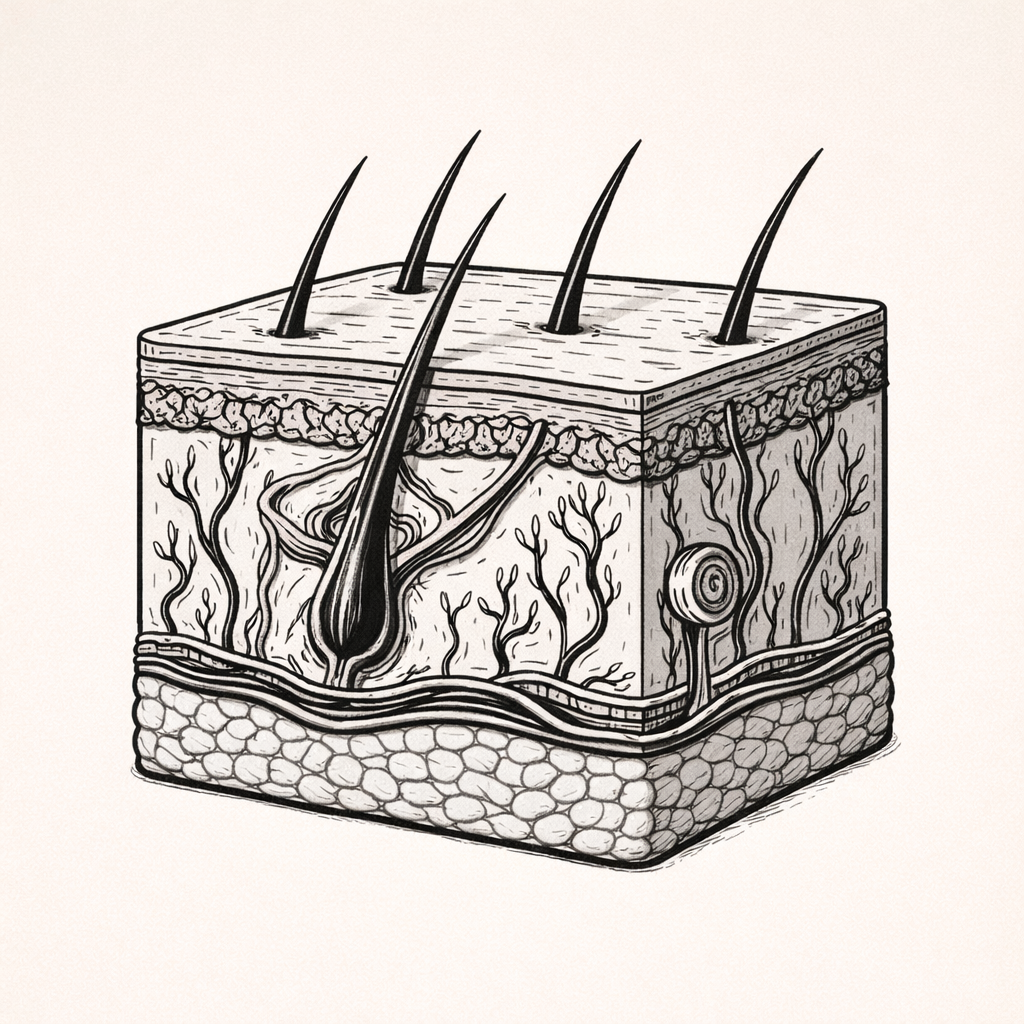
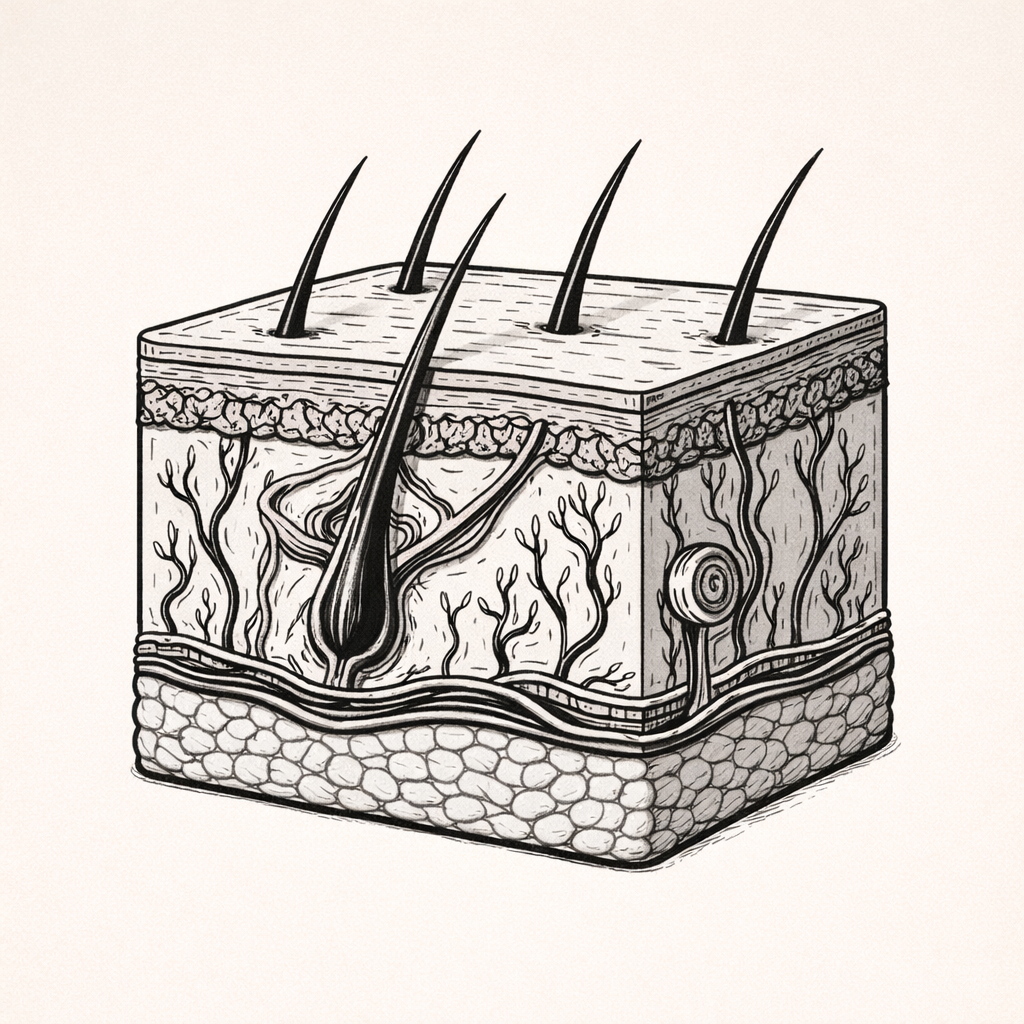
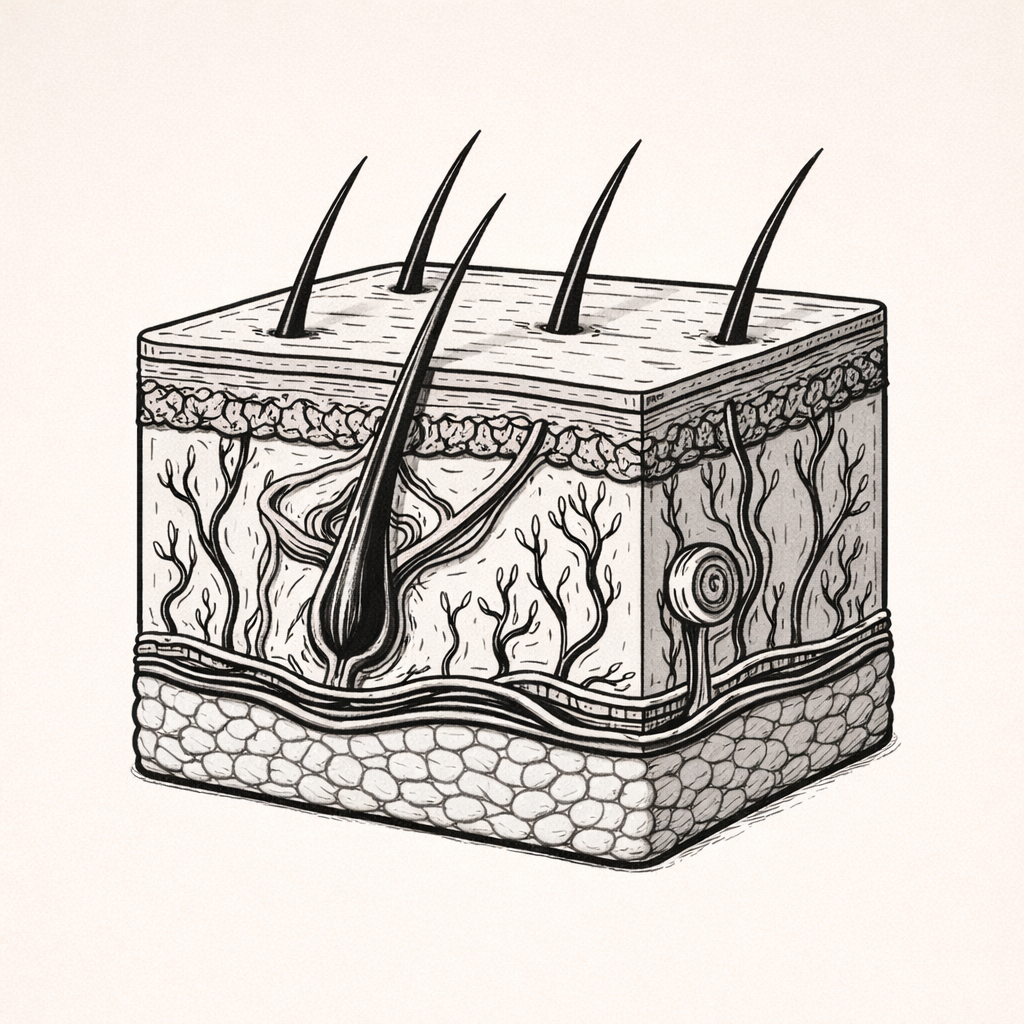
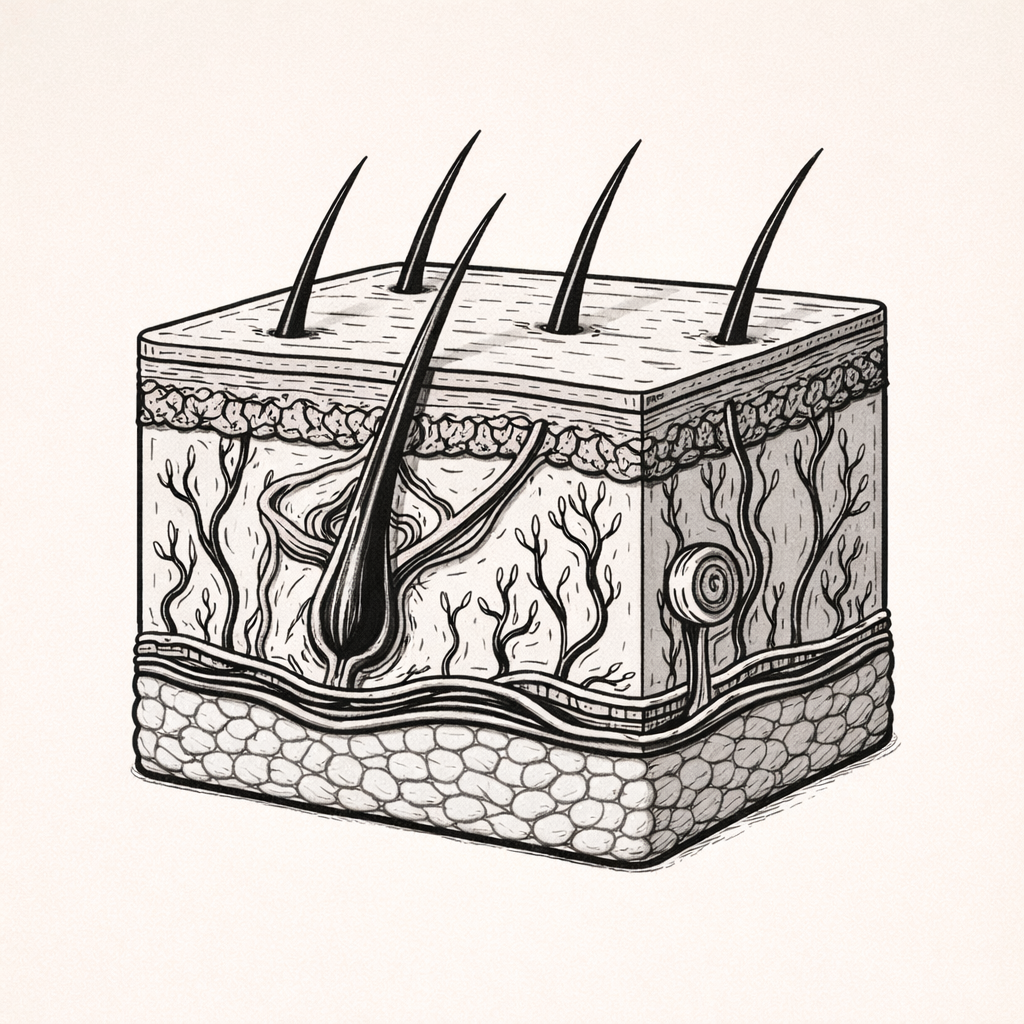
Hair and Hair Follicle Anatomy, Structure & Growth Cycle
Hair and hair follicles are specialised skin structures responsible for hair production, growth cycling, and functional roles such as protection, sensation, and insulation. Understanding their anatomy and growth dynamics is essential for interpreting hair loss, inflammatory follicular conditions, and hormonally driven changes in hair pattern and density.
Nail Anatomy: Structure, Growth and Functional Significance
Nails are specialised keratinised structures that protect the distal digits and enhance fine motor control and sensory function. Understanding nail anatomy and growth is essential for interpreting clinical signs of trauma, infection, systemic disease, and nutritional deficiency.
The Skin Microbiome: Microbial Communities, Protective Functions and Host Interactions
The skin microbiome consists of diverse microorganisms that live on the skin and contribute to barrier protection, immune regulation, and defence against pathogens. Understanding these microbial communities is essential for explaining skin health, wound healing, infection risk, and chronic inflammatory skin conditions.
Thermoregulation: Heat Loss, Heat Conservation and Homeostatic Balance
Thermoregulation describes how the skin contributes to maintaining stable body temperature through heat loss and heat conservation mechanisms. Understanding this function is essential for recognising heat stress, hypothermia, fever, and disorders of autonomic temperature control.
Skin Pigmentation & Melanin: Melanocytes, Melanin Production and Ultraviolet Protection
Skin pigmentation is regulated by melanocytes through the production and distribution of melanin within the epidermis. Understanding how melanin is synthesised and functions is essential for explaining ultraviolet protection, variations in skin tone, tanning responses, and pigment-related skin disorders.
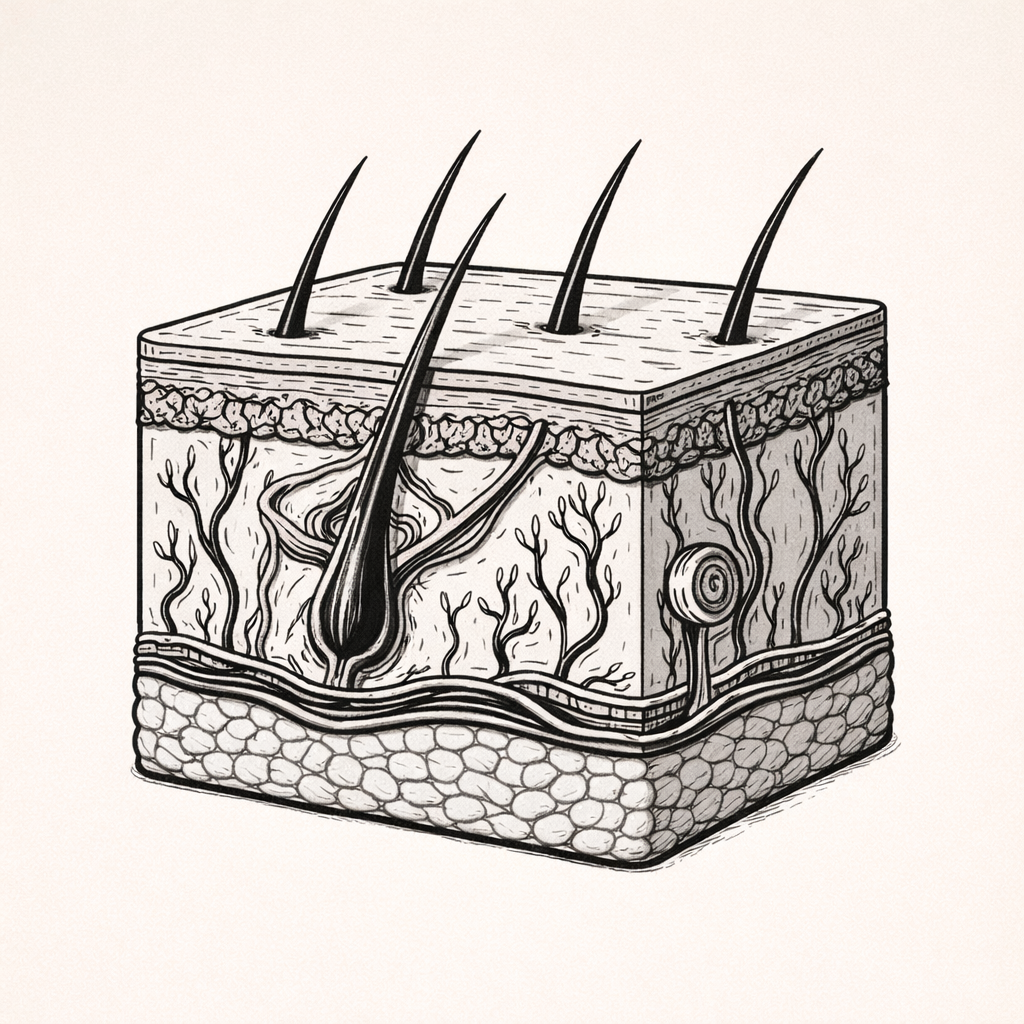
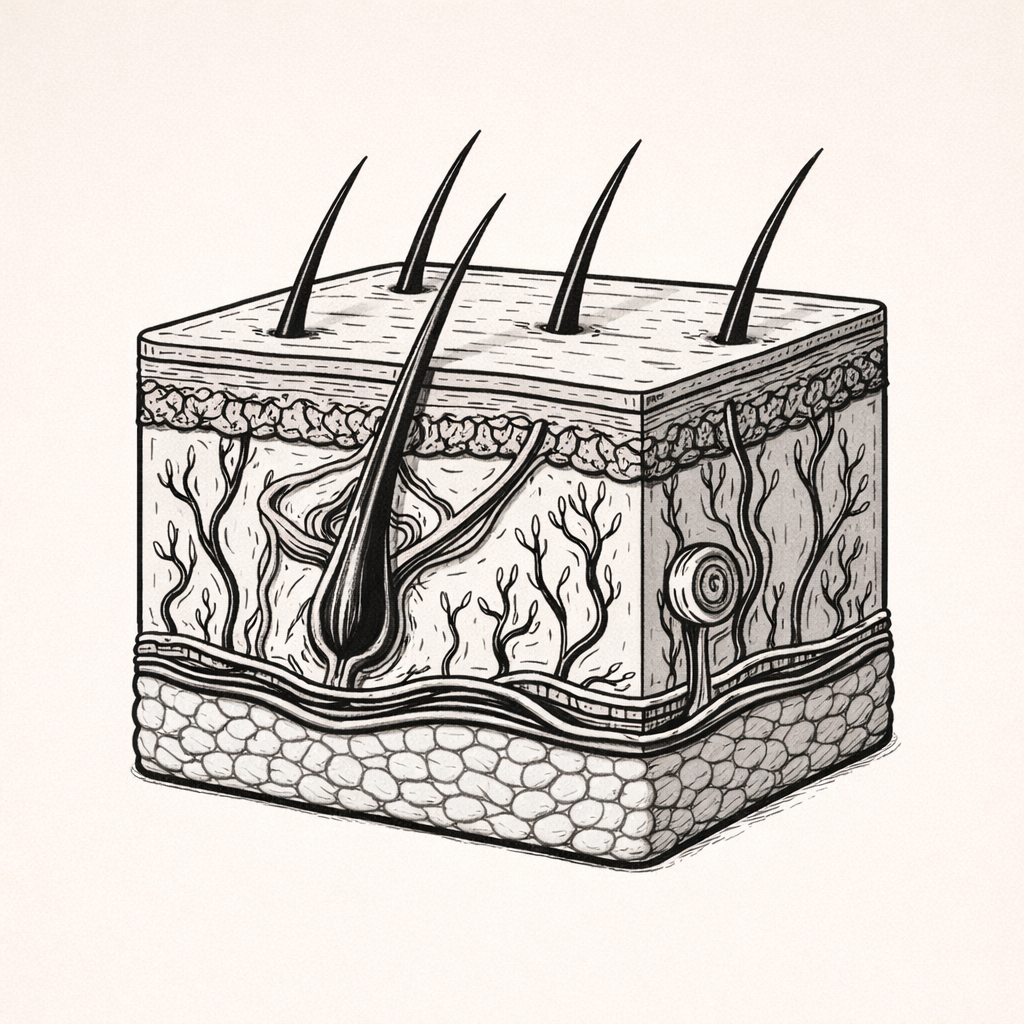
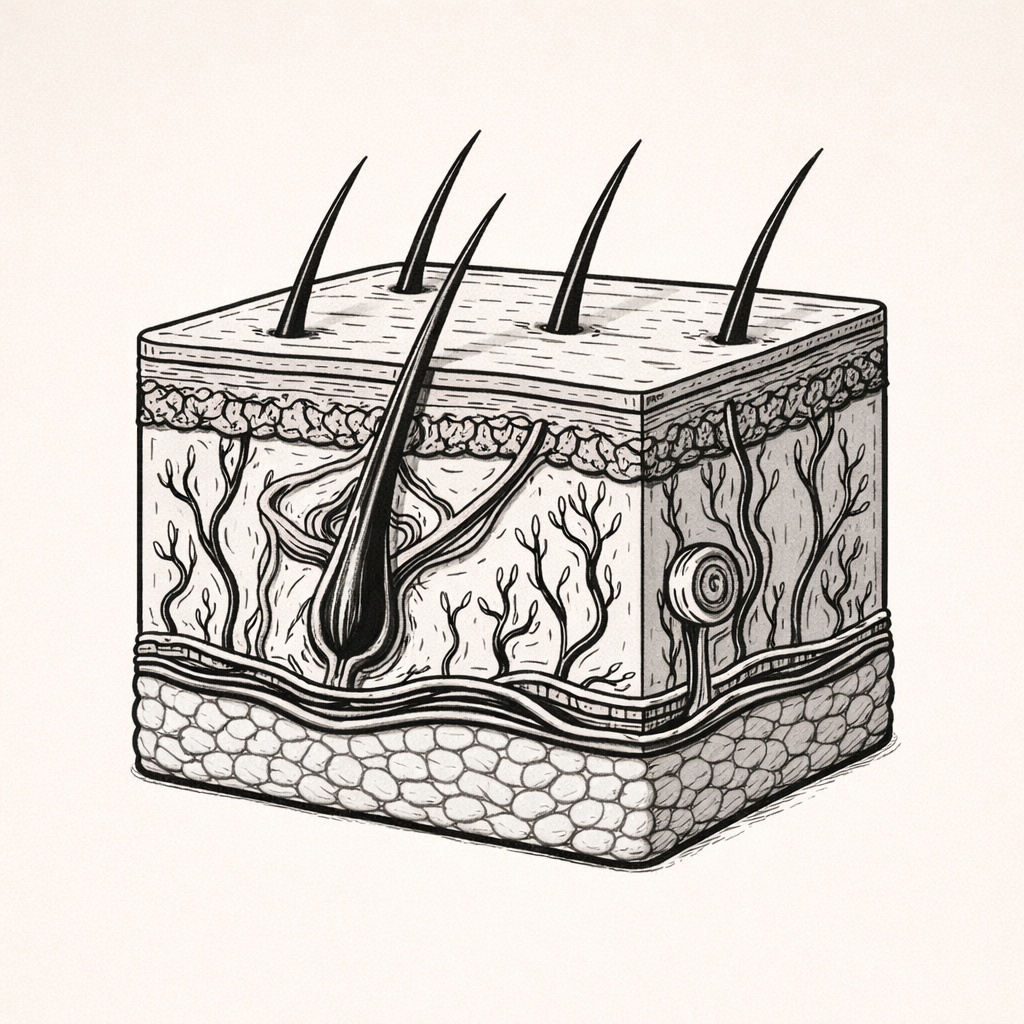
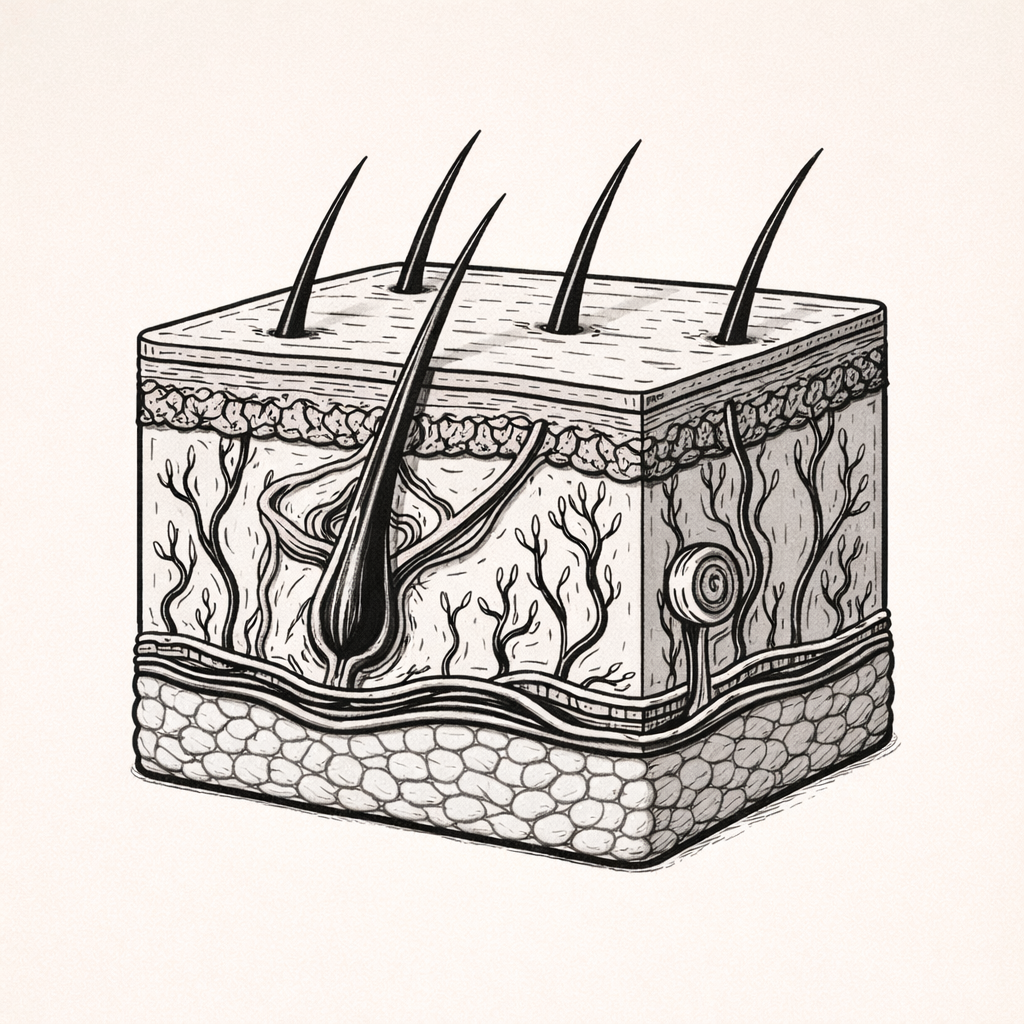
The Integumentary System - Overview
The integumentary system is a complex, multifunctional system that provides protection while regulating temperature, fluid balance, immune defence, sensation, and vitamin D synthesis. Understanding how this system functions is essential for interpreting skin changes, preventing injury, managing wounds, and recognising signs of underlying systemic disease in clinical practice.
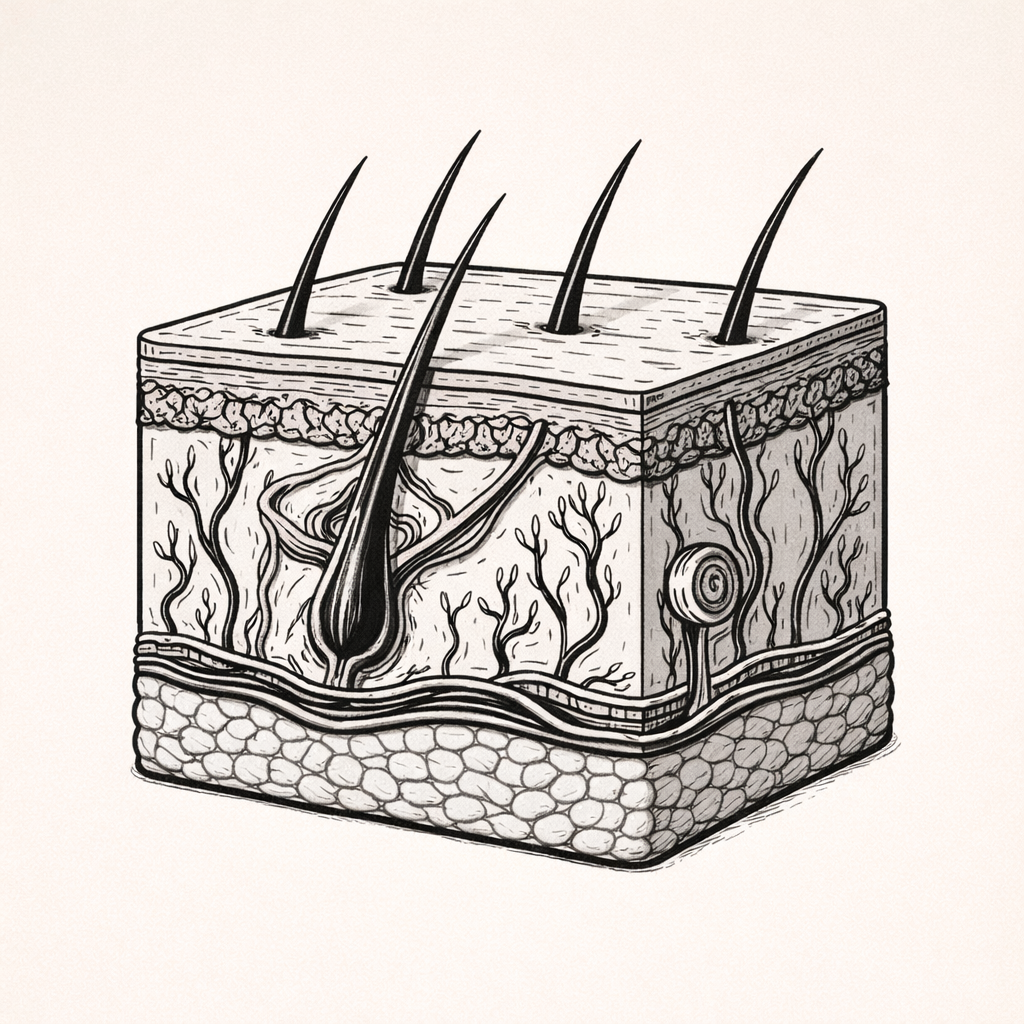
Structure of the Skin Layers: Epidermis, Dermis, and Hypodermis
The epidermis, dermis, and hypodermis are the three structural layers of the skin, each with specialised roles in protection, sensation, thermoregulation, and metabolic function. Understanding how these layers differ is essential for interpreting wound depth, skin pathology, temperature regulation, and systemic disease reflected in the skin.
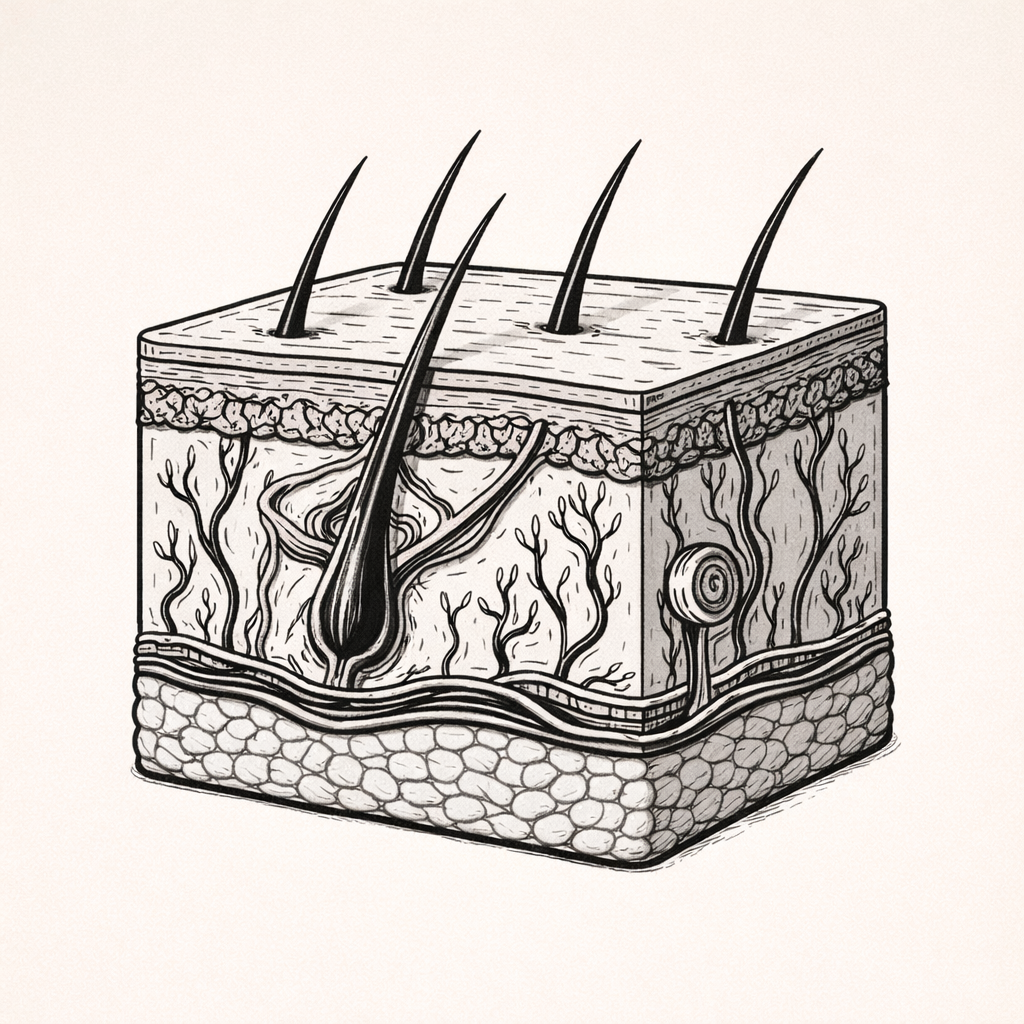
Sensory Receptors of the Skin: Mechanoreception, Thermoreception and Nociception
Sensory receptors of the skin detect touch, pressure, temperature, and pain through specialised neural structures embedded at different skin depths. Understanding how these receptors function is essential for explaining sensation, protective responses, precision movement, and sensory deficits in neurological or skin disease.